
Atrial fibrillation is a term that defines both the location and the nature of one particular type of arrhythmia (abnormal heartbeat). "How Atrial Fibrillation Works" explains what it is and how it forms.
If you have been diagnosed with atrial fibrillation (AF), there are a variety of available treatments to relieve your symptoms and prevent serious complications.
Advertisement
When you are first diagnosed with atrial fibrillation, the doctor may recommend trying to convert the atrial fibrillation back to a normal heart rhythm, a process called cardioversion. You might have to take blood thinners before having cardioversion, especially if there is any concern that you have a blood clot in your heart. Once that's taken care of, your doctor may try cardioversion either through medications or through electricity.
Sometimes, medications are effective in nudging the heart rhythm back to normal. Drugs commonly used for this purpose include amiodarone, dofetilide, disopyramide, flecainide, propafenone, and ibutelide. Many of these drugs have side effects that limit their use in patients with heart failure and other conditions.
If medications fail, the doctor can use electrical energy to "jolt" the heart out of its atrial fibrillation and bring it back to normal. In this procedure, paddles are placed on your chest or on your chest and back. A high-energy electrical shock is sent between the paddles, traveling through the body to the heart. The energy shocks the heart out of atrial fibrillation and back into its normal rhythm.
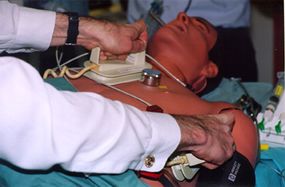
The success of cardioversion, either using drugs or electricity or a combination of the two, depends on how long has been going on, whether there are other abnormalities in your heart, and so on. If cardioversion doesn't work, or if you heart doesn't stay in the normal rhythm, medications can be used to control symptoms and prevent complications arising from atrial fibrillation.
Many of the symptoms of atrial fibrillation arise from the heart beating too fast. Three different types of medications can be used to reduce this rate so that your heart doesn't have to work so hard and you don't have an array of uncomfortable symptoms. They include digoxin, beta-blockers, and calcium-channel blockers. A fourth group of medications, the anti-arrhythmia drugs, might be used to help keep the heart in normal rhythm if cardioversion proves successful.
Digoxin slows the heart rate through the junction between the upper and lower chambers of the heart, thereby preventing all the fast, irregular beats generated in the atria (upper chambers) from reaching the ventricles (lower chambers). This results in a slower heart rate, which means less work for the heart and fewer symptoms for you.
Beta-blockers (carvedilol, propranolol, and many others) not only slow the heart rate, but also directly decrease the workload of the heart, thereby bringing benefits similar to those of digoxin.
Calcium-channel blockers (like diltiazem or verapamil) are also effective in slowing the heart rate.
Anti-arrhythmia drugs (such as amiodarone, dofetilide, and sotalol) can be used to maintain normal heart rhythm and control the heart rate after cardioversion.
The most serious complications from atrial fibrillation can occur when blood clots form in the heart, break apart, and travel to other parts of the body. When these clots lodge in small arteries, they cut off the blood supply. If they lodge in small arteries of the brain, a stroke can result. To prevent these clots from forming in the first place, most patients with chronic atrial fibrillation will be treated with some kind of blood thinner, such as aspirin, a warfarin drug like Coumadin, or a heparin drug like Lovenox. Newer drugs like ximelagatran might also be used in the near future to prevent clots. It's important to take these drugs exactly as prescribed and to have the blood tests recommended by your doctor.
Two types of implantable devices, pacemakers and implantable cardioversion defibrillators (ICDs), are sometimes recommended to help people with atrial fibrillation. These battery-powered devices, about the size of a pocket watch, are surgically placed into the chest. While pacemakers and ICDs are helpful for a variety of heart rhythm disorders, only devices that contain specialized computerized programs for atrial fibrillation can be used in people with this particular rhythm disorder.
For some patients, catheter ablation offers the chance of a cure of their atrial fibrillation. The procedure ablates, or destroys, the tiny areas of heart tissue that are generating the abnormal AF signals. Long, narrow tubes with wires, called electrode catheters, are inserted into the heart to find the diseased area and to apply high-frequency energy to the pinpointed site. Once the tissue is scarred, it is no longer capable of producing atrial fibrillation.
Surgery is the last option and is only recommended when the other treatments have not been effective or when open heart surgery is being performed to correct other problems.
As you can see, there are lots of options for treating your atrial fibrillation. One of these approaches is sure to relieve your symptoms, improve your quality of life, and ensure that you don't encounter serious complications.
Here are some interesting links:
Advertisement