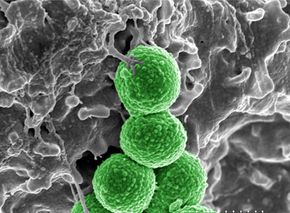
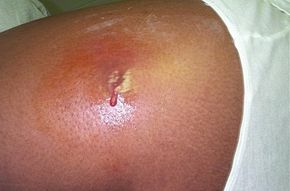
As if you didn't have enough to worry about, now there's the superbug to contend with. No, it's not a giant mantis bent on world conquest. The superbug is a bacterium with a familiar name -- staph. And although this tiny invader doesn't possess 8-foot-long pincers like a giant mantis, it's just as deadly. What's worse, although we could probably take down a giant mantis with bullets -- or possibly rockets -- the superbug becomes harder to kill with each passing day.
It's also getting easier for the bug to kill us. In 2005, 19,000 people died from MRSA infections in the United States, and an average of 6.3 out of every 100,000 infections resulted in death [source: JAMA]. That's more than the number of people who died of AIDS complications in the same year. In the United Kingdom, cases of MRSA increased from 210 cases in 1993 to 5,300 in 2002 [source: University of Warwick].
Advertisement
Methicillin-resistant Staphylococcus aureus, or MRSA (the superbug), was first noticed by physicians in the 1970s. The medical establishment kept an eye on the bug but found it could be killed by a round or two of traditional antibiotics. However, things have changed. Because of improperly taken prescriptions, as well as the presence of antibiotics in our food and water, this staph bug mutated and evolved into the superbug. Due to survival of the fittest, those strains that had lived through an assault of antibiotics went on to breed replicas of themselves. This natural selection eventually led to staph strains that are resistant to these antibodies.
Natural selection is a process of evolution by which those members of a species who live through catastrophe are thought to possess traits that help them survive. Through the survival of those members, these traits -- such as resistance to a disease -- pass from generation to generation. It's the reason you have an opposable thumb: As apes diverged genetically from Old World monkeys 6 to 8 million years ago, one of the results was the opposable thumb. As the thumb showed itself as a "handy" trait, it developed along with the primate family, which includes humans. The results are the human-dominated world we live in today -- thanks, in part, to our opposable thumbs.
The process of natural selection can takes tens (and in some cases, hundreds) of thousands of years to take place in humans. But this isn't the case for MRSA and some other bugs. As the Mayo Clinic put it, MRSA and other bacteria "live on an evolutionary fast track" [source: Mayo Clinic]. Rather than taking thousands of years to develop into their current lethal strain, MRSA has evolved -- and spread -- in mere decades. In 1974, MRSA infections made up two percent of all staph infections. By 2004, MRSA accounted for 63 percent [source: CDC]. What's worse is that this bug has been shown to be fatal in some cases, especially when it remains untreated.
One of the reasons for this is the bacteria's rapidly developing resistance to antibiotics. As its name implies, it's been resistant to Methicillin -- a penicillin-based antibiotic -- for some time now. But it's also showing resistance to other antibiotics, as well, and that has some physicians worried. MRSA can also be easily transferred from person to person, and two types of the bug have developed based on the setting where infection takes place.
So what exactly is this superbug, and just how do we fight it? In this article, we'll look at MRSA, and what -- if anything -- we can do to defeat it.
Advertisement