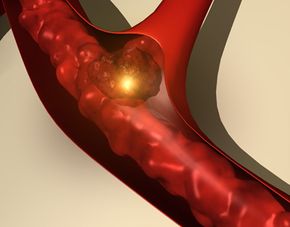
Laser clot busting might sound like something you do in a video game, but you're not likely to see the game Brain Attack at an arcade near you anytime soon. Haven't heard of Brain Attack? Here's how it's played: The goal of the game is to maintain as many points as possible -- points in this game are symbolized by the cells in your brain. You drop your quarter in the game, which leads the enemy, the blood clot, to strike. The clot stops blood flow to the brain, and the brain is instantly deprived of oxygen and nutrients. Now you're going to start losing points -- your brain cells are dying. "Ischemic stroke" the screen flashes. With each lost point, you're losing whatever bodily function that part of the brain controls, be it movement, speech or vision. Time is ticking. What do you do?
If this was a real video game, you might have lots of weapons at your disposal to bust up that clot. But an ischemic stroke, sometimes known as a brain attack, is no game. An ischemic stroke is a type of stroke caused by a blood clot. Time is still of the essence so that brain cells can be saved and brain damage minimized. But right now, there's only one weapon in a doctor's clot-busting arsenal. That weapon is tissue plasminogen activator, or tPA. The drug tPA was approved by the FDA for use in 1996. It's intravenously administered and it works to dissolve the clot so that blood can flow again.
Advertisement
But for being a doctor's major weapon in a brain attack, tPA is very rarely used. Only one in five patients that could benefit from the drug actually receives it [source: Brody]. The drug only has a three-hour window in which it can be administered after symptoms of a stroke start to appear, and many patients simply don't make it to the hospital in time. After that window, tPA may cause bleeding in the brain.
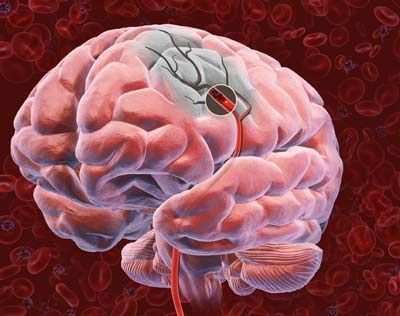
Scientists are studying several new treatments for stroke that could both elongate that treatment window and break up the clot faster. One of those methods is laser clot busting, which despite its video game-ready name, would actually be more akin to a game of Operation. In the game Operation, players try to extract organs, bones and other items without touching the sides of a bodily cavity. In laser clot busting, doctors would be trying to bust up a clot without breaking the surrounding blood vessel.
Turn the page to find out more about how this treatment might work.
Advertisement