Just as computers revolutionized the latter half of the 20th century, the field of robotics has the potential to equally alter how we live in the 21st century. We've already seen how robots have changed the manufacturing of cars and other consumer goods by streamlining and speeding up the assembly line. We even have robotic lawn mowers and robotic pets. And robots have enabled us to see places that humans are not yet able to visit, such as other planets and the depths of the ocean.
In the coming decades, we may see robots that have artificial intelligence. Some, like Honda's ASIMO robot, will resemble the human form. They may eventually become self-aware and conscious, and be able to do anything that a human can. When we talk about robots doing the tasks of humans, we often talk about the future, but robotic surgery is already a reality. Doctors around the world are using sophisticated robots to perform surgical procedures on patients.
Advertisement
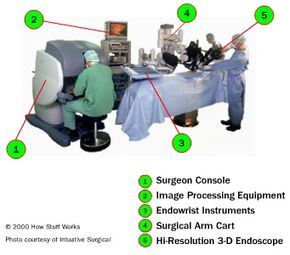
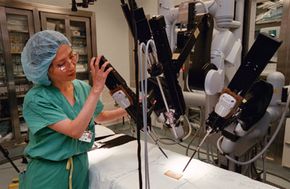
Not all surgical robots are equal. There are three different kinds of robotic surgery systems: supervisory-controlled systems, telesurgical systems and shared-control systems. The main difference between each system is how involved a human surgeon must be when performing a surgical procedure. On one end of the spectrum, robots perform surgical techniques without the direct intervention of a surgeon. On the other end, doctors perform surgery with the assistance of a robot, but the doctor is doing most of the work [source: Brown University].
While robotic surgery systems are still relatively uncommon, several hospitals around the world have bought robotic surgical systems. These systems have the potential to improve the safety and effectiveness of surgeries. But the systems also have some drawbacks. It's still a relatively young science and it's very expensive. Some hospitals may be holding back on adopting the technology.
Why would a hospital consider a robotic surgery system in the first place? Find out in the next section.
Advertisement