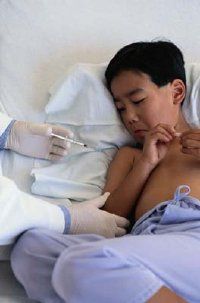
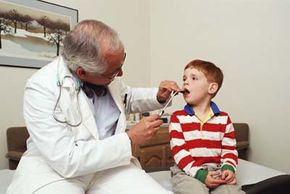
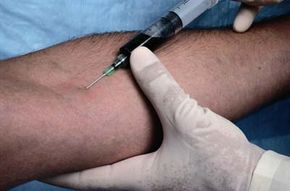
Children are born with temporary protection from many diseases, thanks to antibodies from the mother passed through the placenta. Within a year, however, this defense is lost and a number of illnesses come knocking at the door.
Childhood vaccinations protect us from these diseases, but when they aren't complete, the bugs come crawling back. In this article you'll find helpful information on the following vaccines:
Advertisement
- Chickenpox Vaccine. Anyone born before the 1990s probably remembers the agony associated with those small red bumps fondly known as chickenpox. Thankfully, a vaccination was developed in 1995, and now almost all children receive a vaccine between the ages and 12 and 18 months. What's more, even if a vaccinated child comes down with the chickenpox, the severity of the disease will be significantly decreased. Find out even more about the chickenpox vaccine on this page.
- Diphtheria Vaccine. Children usually receive the diphtheria vaccine as part of an immunization for diphtheria/tetanus/pertussis -- DTP or DTaP. Without this vaccination, a child who develops diphtheria may exhibit symptoms such as breathing problems, double vision, heart rhythm problems, and more. Learn as much as you can about diphtheria in this section.
- Rubella Vaccine. Rubella, or the German measles, is also known as the "three-day measles" because the duration of this illness is usually quite short. Don't let this fool you, though. Getting your child immunized for rubella is important. This vaccine is typically given in the form of a measles/mumps/rubella (MMR) immunization. Learn more on this page.
- Flu Vaccine. It's just the flu...how bad can it be, right? Wrong! There is a strain of the flu, called invasive H. flu, that is particularly dangerous for young children. Thankfully, there is a vaccine available today to protect them against this infection. Learn about it and about the symptoms of invasive H. flu here.
- Measles Vaccine. Measles is a viral infection that affects the respiratory system. It starts out with symptoms similar to the common cold, but this disease can actually be fatal. Find out how to protect yourself and your family against the measles on this page.
- Mumps Vaccine. While the mumps is not as potentially harmful as other infections like measles, it can be dangerous, especially if the swelling caused by the virus reaches the brain or other organs. Learn more about the mumps vaccine as well as other preventative measures you can take to avoid it.
- Polio Vaccine. Before the polio vaccine was introduced in 1955, polio was a frightening disease that left some young children paralyzed. Thanks to the vaccine, there are few, if any cases reported in the United States today, but it is still important to know the signs of this disease and why it's so important to get immunized. Find out more here.
- Shingles Vaccine. Shingles is an often painful infection that is caused by the varicella-zoster virus -- the same one that contributes to chickenpox. This disease is more prevalent among people age 50 and older who have weakened immune systems. Learn about the shingles vaccine as well as the symptoms to watch out for.
- Tetanus Vaccine. Many people think you can only get tetanus, or lockjaw, from stepping on a rusty nail, but there are other ways to contract this disease. Because of this, it's so important to stay on top of you tetanus vaccine and know what signs to look out for. See this section for details.
- Whooping Cough Vaccine. Whooping cough causes a child to suffer from coughing spells that have a distinctive cough that ends with a "whooping" sound. It typically affects children under one, but others are susceptible if their immunizations are not up to date. Find out more about whooping cough on this page.
Advertisement