When you want to get pregnant, every month that passes without a positive pregnancy test can seem like a lifetime. After all, more than 6 million American women get pregnant every year, so what's the problem [source: National Vital Statistics System]? The culprit is often impaired fertility, and one out of every six couples trying to get pregnant has trouble conceiving after a year of unprotected sex. About half of those couples will go on to conceive the old-fashioned way or with very minimal help, but the other half? The other half may find themselves struggling with conception or with carrying a pregnancy to term; these couples may need more testing and advanced fertility treatments [source: Taylor].
Fertility problems might manifest for a variety of reasons in both women and men, from health problems such as hormonal imbalances to habits such as smoking. Age is an important factor, as is diet and weight. But sometimes the reason why a woman can't get pregnant or isn't successful carrying a pregnancy to term has no explanation -- as many as 20 percent of couples with fertility problems never know the cause [source: Newton-Wellesley Hospital].
Advertisement
And then there are conditions that may or may not affect your fertility. One of those is adenomyosis.
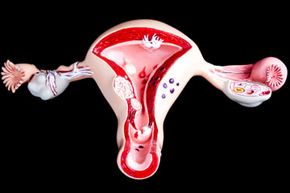
Adenomyosis is what's called a structural gynecological disorder, just as fibroids, polyps and endometriosis are structural disorders (opposed to hormonal imbalance or inflammation) that could affect the reproductive system. It affects the endometrial cells in the lining of the uterus and the muscular layer of the uterine wall.
In theory, adenomyosis is a condition that can affect a woman's fertility if it develops during her childbearing years, but research is still preliminary, and questions about the impact of the condition on conception rates and pregnancy risks currently remain unanswered. Let's dive a little deeper into the cause and symptoms of adenomyosis.
Advertisement