Countless procedures and applications of topical exfoliating creams are supposed to remove and prevent skin flaws. But leave it to stubborn dead cells to find a way around your smooth skin routine, turning your face into a sea of pinpoint-sized bumps. In fact, your very diligent skin care plan may be at fault -- it can actually traumatize your skin and make you a prime candidate for milia.
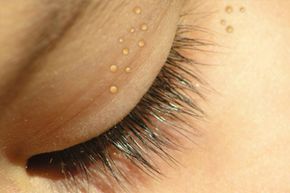
Milia are raised, whitish bumps on the skin that commonly appear on infants after birth, but adults can get them too. The miniscule, pimple-like cysts appear because dead skin cells are trapped in the surface of the skin or mouth [source: University of Maryland Medical Center]. The primary form of milia generally goes away on its own in both infants and adults. Adults, however, may also experience milia's secondary form, which requires some medical attention.
Advertisement
Cysts caused by dead skin cells can develop after blistering skin rashes, or they can arise from existing chronic skin disorders [source: American Osteopathic College of Dermatology]. But simple things like exfoliating creams, abrasive skin treatments and sun exposure can cause enough irritation to trigger a case of milia.
In children, since there is minimal skin trauma at birth, the bumps almost exclusively appear on the face. Milia in adults can appear anywhere that there are sweat ducts. These areas may be affected and blocked because of excessive skin irritation or pore-clogging rituals.
Milia appear topical and small, but -- especially with the secondary kind -- experts say the problem can be deeper. If you don't see a specialist to determine whether you have primary or secondary milia, you could be doing more harm to your skin if you try to remove them at home. Without the right tools -- like those used in a doctor's office -- secondary milia are difficult to remove and can lead to scarring [source: Skin Sight].
Read on for more details about why the bumps appear in the first place, and what you can do to prevent milia and the side effects of this condition.
Advertisement