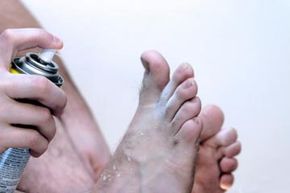
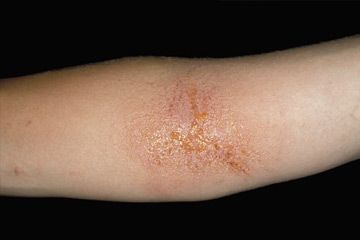
It feels like something out of a scary movie. Your toes begin to itch. You feel something burning in your shoes. You scratch, but it doesn't help. Soon, you notice blisters. The skin between your toes starts to crack. You find that the soles of your feet are starting to peel. You apply lotion, but nothing seems to help. You start to think your toenails are changing color, and you eventually suspect that the itchy, burning feeling is spreading to other parts of your body. What is happening to you? Are you being taken over by an alien life form?
The answer is likely much simpler. You have athlete's foot, known to your doctor as Tinea pedis. And though it might feel like you're being attacked by an invader from outer space, what you're experiencing is actually a very common infection that can be caused by a number of persistent -- though most definitely earthbound -- critters.
Advertisement
Athlete's foot is one of a number of related skin conditions with similar names: Tinea corporis, Tinea capitis (scalp ringworm) and Tinea cruris (jock itch). Of these conditions, athlete's foot has perhaps the least frightening name. But it can be just as uncomfortable as its icky-sounding cousins and just as difficult to get rid of [source: Mayo Clinic].
Athlete's foot, in addition to the other Tinea conditions, is caused by fungi. That's why some people more casually call the condition "foot fungus." As with any fungus, the one that results in athlete's foot likes a warm, humid environment. Think about how quickly a fresh loaf of bread gets moldy in the heat and humidity of summer. For many people, the sole of the foot and the spaces between the toes are both warm and moist. It's the perfect condition for sprouting a batch of fungus.
If you've got a fungus you need to foil, continue reading to learn what causes this irritating invasion and how you can defeat your athlete's foot.
Advertisement