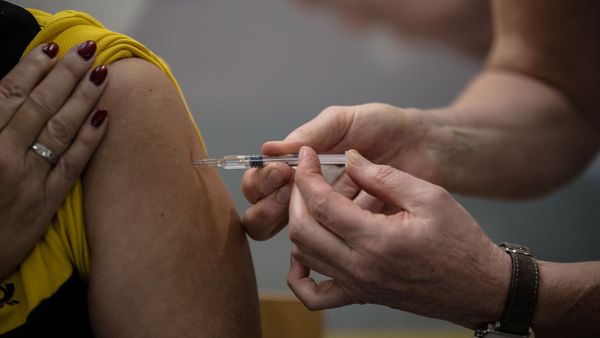
Nobody likes to be sick, but it seems there are plenty of people who are willing to take a chance on a disease like COVID-19, instead of getting a vaccine. Why is that? And is this a new phenomenon? First, we have to understand the difference between vaccine hesitancy and anti-vaccine activism (or vaccine resistance).
"Vaccine hesitancy and anti-vaccine activism are distinct and largely unrelated," explains Noel Brewer, Ph.D., professor of health behavior at the University of North Carolina in an email. "Only around 2 percent of Americans will never get a vaccine, and among these hard refusers only a handful attempt to recruit others to their views."
Advertisement
By comparison, he says, most people have at least some questions about vaccines, which is not a bad thing. "Vaccine hesitancy is normal and healthy and should be encouraged. It's good to have questions, ask them and get high-quality, trustworthy answers," he says.
The vocal anti-vaccination movement is fairly recent and was really kicked into gear in 1998 by a now-discredited paper that appeared in the medical journal Lancet linking vaccines and autism, says Brewer. However, vaccine hesitancy is as old as vaccines themselves.
Advertisement