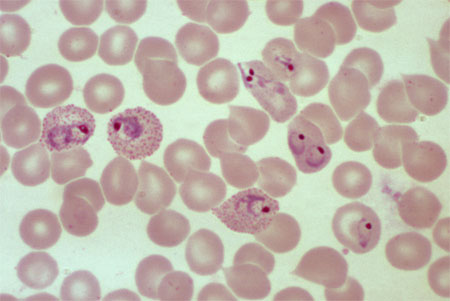
Malaria is an infection transmitted by a certain type of mosquito. Eradicated in the United States and other developed countries, it is now a disease of tropical areas in Africa, Asia, Central and South America, the Middle East and Oceania. Today, malaria is widespread in more than 100 countries, affecting about 300 million people and causing 1 million deaths a year. More than 90 percent of cases occur in tropical Africa, with young children and pregnant women making up most cases. In Africa, malaria is the leading cause of death for children under the age of five.
Globally, more than 2 billion people are at risk for malaria, with the majority of cases occurring among the poorest 20 percent of the world's population. In these poor and often rural areas, healthcare systems are inadequate and sanitation is poor. Increasing resistance to the drugs used to treat malaria and insecticides used to prevent it also contribute to the growing prevalence of the disease and to its resurgence in areas where it had been eliminated.
Source:Roll Back Malaria Partnership
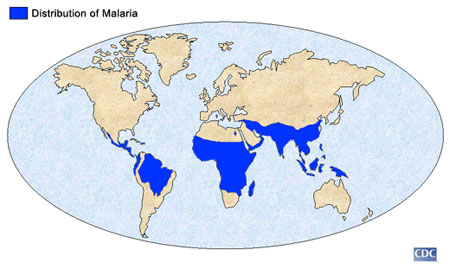 Photo courtesy CDC The geographic distribution of malaria |
Causes of Malaria
Malaria is caused by parasitic, single-celled organisms called Plasmodium. Like the Avian flu, malaria is a vector disease, in which the infecting organism is transported by an intermediary animal carrier. In the case of malaria, the disease is transmitted by mosquitoes -- but only by female mosquitoes of the Anopheles genus.
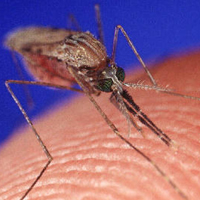 Photo courtesy Jim Gathany/CDC A female mosquito (Anopheles gambiae), feeding |
The mosquito picks up the parasite when it bites and extracts blood from infected people. The parasites reproduce while the mosquito uses the blood to nurture her eggs. When the mosquito bites a human again, the parasites are passed into that person's blood. Once inside the body, the parasites multiply rapidly in the liver and in red blood cells. From there, the parasites may invade other organs, including the brain.
Malaria can be transmitted from human to human by transfusion of infected blood and by contaminated syringes and needles. In areas where the disease is common, people are infected so frequently that they develop a degree of acquired immunity and have no symptoms. They may unknowingly spread the disease through blood. Pregnant women can also pass the parasites during pregnancy or birth.
We'll learn about the symptoms, diagnosis, treatment and prevention of malaria in the next section.
|
|
Advertisement