Choosing the proper health insurance plan is a huge decision for most families. There used to be one type of service (now known as a fee-for-service plan), but since then we've been bombarded by choices. Today, trying to find the best plan for you or your family is enough to make you reach inside your medicine cabinet. You need to know what options are available to you, what each of those options offers and whether or not you can afford them. In this article, we'll look at the two primary issues that most people face when trying to find the right health insurance plan: budget and need.
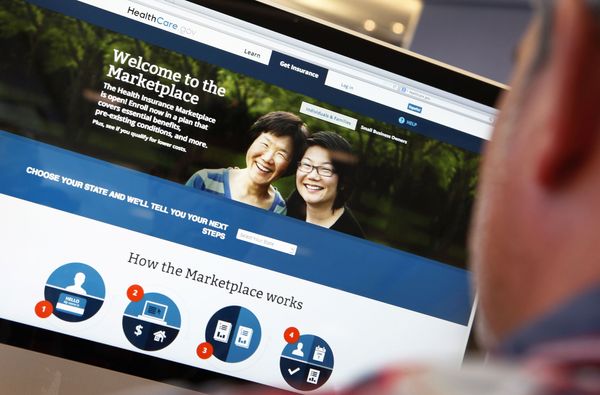
Keep in mind that there is no one-size-fits-all health insurance plan. To find out what kind of coverage you need, and to avoid paying for what you don't, there are several questions you should carefully consider before you sign on the dotted line. Once you've settled on a plan, it's your responsibility to thoroughly understand it and follow its guidelines. The variety of plans seems endless, so where do you begin to make sense of them all? There are several key factors to consider when purchasing a health care plan -- we'll wade through these factors to help you find out how to choose the best one for you and your family.
Advertisement
Finding the intersection of budget and need can be tough. The needs of a healthy twentysomething are vastly different from the needs of a family of four, which are vastly different from a baby boomer entering retirement. Luckily there are good options for each situation. Every kind of health insurance plan, be it a managed-care or fee-for-service plan, has different ways of handling every different kind of scenario. First, you need to determine what kind of coverage you need and whether or not you can afford it.
Let's take a look at the questions raised by finances. Those of us who are operating under a low financial ceiling need to pay careful attention to where our health care dollars are going. Do you visit the doctor very often? How much of a monthly premium can you afford? Can you meet your deductible in order to get full coverage? If you choose a managed-care plan, how much more will it cost to go out of the provider network? Is there a limit to the amount you'll have to pay and to the amount paid to you by your insurance carrier?
Of course, these financial concerns are made doubly important when you begin to factor in your own health care needs. Are you caring for any dependents? Do you have any pre-existing conditions? How comprehensive do you want your plan to be? Do you need dental and vision plans? Do you have a chronic illness that requires monthly treatment? What are your month-to-month medical expenses, like prescription drugs? What could happen should you require surgery? What if you were injured in an accident? How much preventative care do you want?
These are tough questions, but it's never a good idea to bury your head in the sand, especially where health is concerned. With careful consideration of these questions, you and your family will be able to find that health care sweet spot -- where you get the coverage you need at prices you can afford.
In the next section we'll dissect each of these plans.
Advertisement