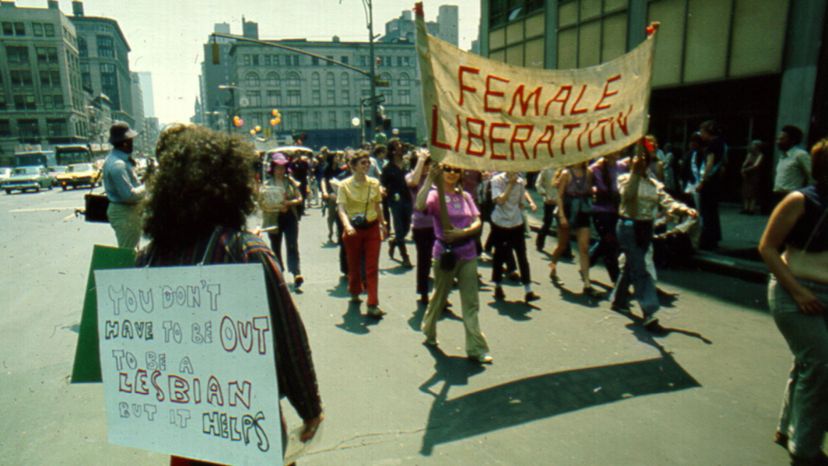Before the 1970s, homosexuality was often considered a mental illness. Indeed, the American Psychiatric Association (APA) classified it as such in its first Diagnostic and Statistical Manual of Mental Disorders (DSM), published in 1952. This was not a controversial position at the time — it held with prevailing norms. But then gay activists started protesting at annual meetings of the APA, and presented scientific evidence opposing this view.
In 1973, it was put to the vote and the majority (58 percent) of APA members agreed homosexuality should no longer be considered a mental disorder [source: Group for the Advancement of Psychiatry]. This change was a huge step for gay rights and helped to shift societal thinking on homosexuality. It also demonstrated the power of the DSM, the diagnostic manual of the APA, on public opinion.
Advertisement
Now in its fifth edition and known as DSM-5 (this is the first edition without a Roman numeral), the publication does not offer treatment or medication advice for the 157 disorders described in its pages. Rather, it was designed to help healthcare professionals better identify and diagnose mental disorders, such as those that impact personality, cognition, mood and identity. The manual also provides uniform diagnostic codes for each issue, which are used to facilitate billing and data collection [source: APA]. Often, if a condition is not listed in the DSM, U.S. health insurance companies won't pay for treatment for it.
The manual is primarily used in the United States, with much of the rest of the world's health professionals turning instead to the World Health Organization's (WHO) International Classification of Diseases (ICD), which covers all diseases, not just those psychiatric in nature. APA encourages healthcare professionals to consider DSM-5 and ICD as "companion publications," designed to be compatible with each other.
So how did it start? The DSM was developed in response to an obvious need for mental illness classification systems. The U.S. Census of 1840 took baby steps toward the eventual development of the manual when it added incidents of "idiocy/insanity" to its survey. This was possibly the first attempt at statistical information-gathering related to mental illness, and therefore a pretty big deal. In 1880, the Census fleshed out the mental health categories to include issues like dementia, melancholia, epilepsy and mania [source: APA].
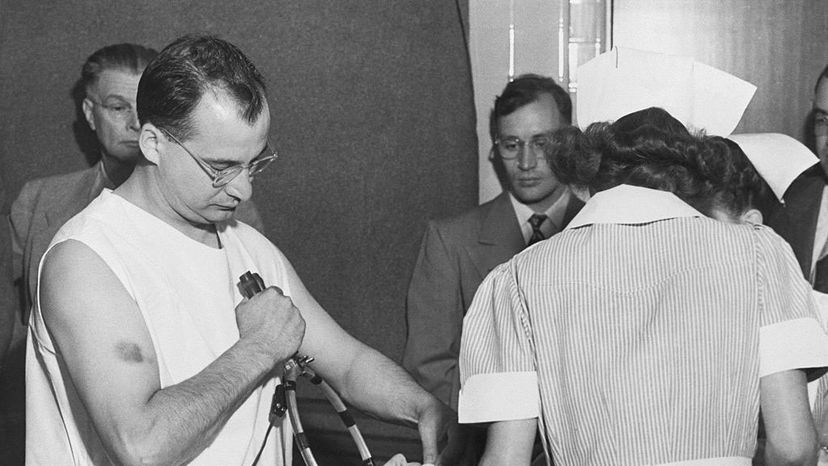
Mental institutions of the past have been the stuff of horror movies, a fate sometimes worse than death for those who wound up behind their walls. Just a century ago, people were institutionalized for relatively common, now-treatable problems, like bipolar disorder [source: Mental Health America]. Fortunately, mental illness detection, treatment and diagnosis, although still far from perfect, have come a long way. One of the measures credited with improving care quality was the development of the DSM.
In 1917, the American Medico-Psychological Association (the forerunner of the APA) and the National Commission on Mental Hygiene came up with a plan, adopted by the Census Bureau, for gathering uniform health statistics in mental hospitals. And in 1921 the APA started to develop psychiatric classifications for various severe psychiatric disorders. After World War II, the APA used a bigger classification system developed by the U.S. Army as it was treating veterans to develop the first DSM [source: APA].
Advertisement