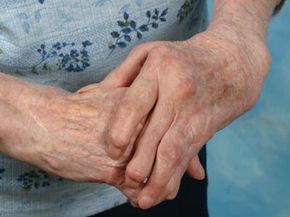
Many of us think of arthritis as a condition that causes old people to rub their hands together and predict changes in the weather. That's not entirely the case. In fact, there are some truths about arthritis that may surprise you. For starters, arthritis isn't just one disease -- there are more than 100 types of arthritis. More than 350 million people worldwide have arthritis, as nearly one in five Americans [source: Shiel]. And it affects younger people, too -- six out of 10 arthritis sufferers are under 65 years old [source: CNN].
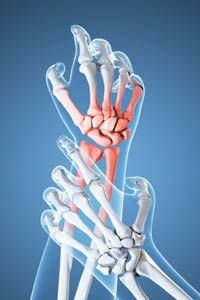
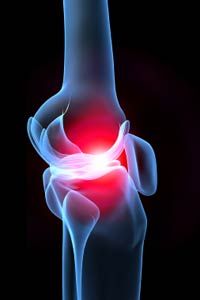
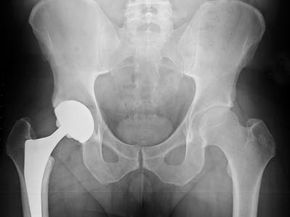
So, what exactly is arthritis? Arthritis is swelling in one or more of your joints that causes pain and stiffness and can lead to destruction of tissue in the joint. In some cases, a joint can become so damaged that it needs to be replaced, as is often the case with osteoarthritis (an age-related form of arthritis) and hip joints.
Advertisement
There are different causes of this inflammation, which we'll discuss throughout this article. Arthritis can be caused by genetics, an old ski injury or your own immune system. You may first experience discomfort late in life, or you could be diagnosed when you're just a teenager.
Joint pain touches every part of a person's life. Not only do your activity levels plummet, you end up spending more and more time just managing pain. Physical abilities are curbed and independence can be compromised or even entirely lost.
There are many therapies and drugs available for the treatment of arthritis, and arthritis research continues to turn up new treatment options. As our understanding of arthritis grows, we'll be better able to recognize its early symptoms, seek out the right kind of help and retain -- or reclaim -- as much of our pre-arthritic lives as possible.
Advertisement