Of all the forms of cancer, pancreatic is one of the most dreaded diagnoses. This reputation is earned, unfortunately, as the 5-year survival rate for pancreatic cancer is just 10 percent, according to the American Cancer Society. That number represents an improvement, however, over the 2011 five-year survival rate of 6 percent.
Although the disease has publicly affected icons like "Jeopardy!" host Alex Trebek and Supreme Court Justice Ruth Bader Ginsberg, most people still have a pretty limited understanding of it. So, how is it that cancer of such a small organ can cause so much trouble? And why is the survival rate so low?
Advertisement
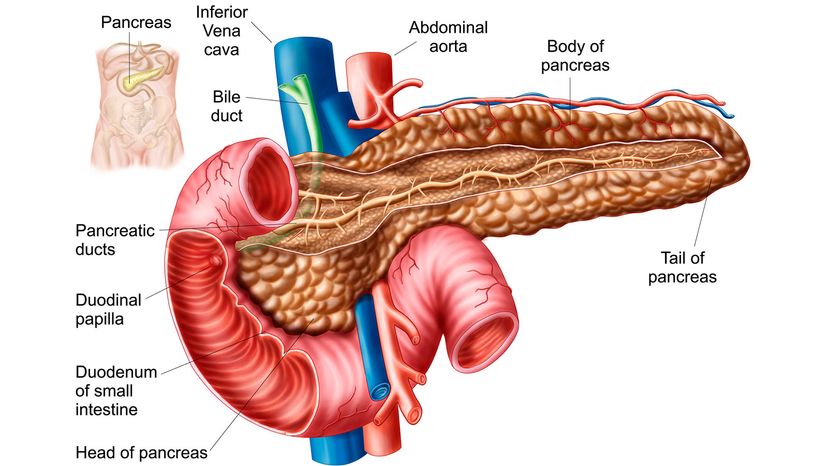
First, it's important to have a grasp on where the pancreas is, and what it does. Only about 6-10 inches (15-25 centimeters) long, the pancreas sits in the upper left abdomen behind the stomach, and is surrounded on all sides by other, more prominent organs like the liver, small intestine and spleen. Although small in size, the pancreas has some mighty functions, like creating and dispensing hormones that regulate blood sugar, as well as enzymes that help the body digest proteins, fat and carbohydrates. When the pancreas gets out of whack, health tends to decline pretty quickly.
Advertisement