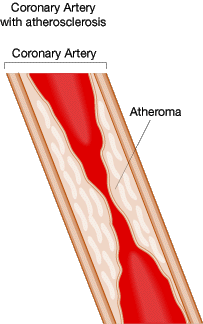
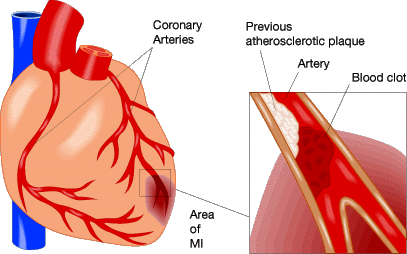
There are many risk factors that increase the likelihood of developing atherosclerosis and CAD. These include:
- hypertension (high blood pressure)
- diabetes
- elevated cholesterol
- smoking
- sedentary lifestyle
- stress
- obesity
- male sex
- family history of heart disease
- older age
Obviously, some of these risk factors can be changed or controlled (on your own or with the help of your physician) and some cannot. And, some of these risk factors have an effect on each other. For example, many people can lower their blood pressure by simply giving up smoking. Also losing weight can help:
- control blood sugar in diabetes
- lower blood pressure
- lower cholesterol
Age, Sex, Family history
You cannot control your age, family history, or gender. However, you can use these risk factors as impetous to take control of those risk factors you can change. Because heart disease is more common as we age, it is even more important to pay attention to your weight, blood sugar, cholesterol levels, blood pressure and exercise regimen. Men, in general, are at increased risk for coronary artery disease. When women reach menopause and the protective effect of the estrogen hormone is lost, the risk among genders becomes equalized. Keep in mind that while estrogen replacement may reduce a woman's risk of heart disease, there's a slightly increased risk of some cancers. Also, CAD is more common if you have a close relative (mother, father, sibling) who has had CAD at an early age.
Hypertension
Hypertension (elevated blood pressure)is a risk factor for CAD. Hypertension can also lead to strokes, kidney disease, and aneurysms. Also, hypertension causes the heart to work harder and can lead to Congestive Heart Failure. Your blood pressure (BP) has two numbers. In a blood pressure reading, the upper number is called the systolic blood pressure. A systolic BP less than 140 is considered normal. The lower number is called the diastolic BP. A diastolic BP less than 90 is considered normal. Blood pressure that is slightly higher than this is called mild hypertension and can sometimes be reduced by weight loss, cessation of smoking, and decreased salt intake. However, medications may sometimes be necessary. There are six classes of medications to treat hypertension. These are:
- Diuretics - Also known as "water pills" these medications -- such as hydrochlorothiazide and furosemide -- excrete extra water and salt to lower blood pressure.
- Anti-Adrenergic drugs - Commonly called alpha and beta blockers, include medications such as Prazosin, Terazosin, Doxazosin, and Propranolol, Metoprolol and Atenolol. These block a part of the nervous system that increases blood pressure.
- Vasodilators - Medications such as Hydralazine and Minoxidil work by relaxing blood vessels to lower blood pressure.
- ACE (angiotensin converting enzyme) inhibitors - These medications work by dilating (enlarging) blood vessels by preventing the production of angiotensin which is a vasoconstrictor (blood vessel constrictor). Some commonly prescribed ACE inhibitors are Captopril, Enalapril, Lisinopril and Benazepril.
- Angiotensin receptor antagonists - Medications such as Losartan and Valsartan are similar to ACE inhibitors and block the effects of angiotensin instead of preventing its production.
- Calcium channel blockers - Because they block the calcium flow into cells which is needed to constrict blood vessels, medications such as Diltiazem, Verapamil, and Nifedipine work by dilating blood vessels.
Smoking
Smoking leads to CAD as well as many other illnesses such as COPD (chronic obstructive pulmonary disease which includes emphysema, asthma and chronic bronchitis). It also causes lung cancer, strokes and many other illnesses. Smoking may increase atherosclerosis as well. The nicotine in cigarettes causes constriction in blood vessels which causes an increase in blood pressure thereby causing the heart to work harder. Furthermore, nicotine may constrict coronary arteries and reduce blood flow to the heart muscle.
There are many ways to stop smoking. Usually it is best to quit completely either by yourself or with the help of support groups, along with the use of nicotine gum or a nicotine patch.
Elevated cholesterol
There is a definite relationship with elevated cholesterol and CAD. Cholesterol is transported in the blood by lipoproteins. Two of these lipoproteins are low density lipoprotein (LDL) and high density lipoprotein (HDL). An elevated level of LDL (the bad cholesterol) is associated with an increased risk of CAD. An elevated level of HDL (the good cholesterol) is associated with a decreased risk of CAD. Cholesterol levels can be lowered by eating a diet low in meat, eggs and dairy products. However, most of the cholesterol in the blood is produced in the liver. If a low fat diet does not sufficiently reduce your cholesterol, then your physician can prescribe medications to do so. There are four classes of medications that lower cholesterol:
- Bile acid binding resin medications, such as cholestyramine and cholestipol, bind bile salts and prevent their reabsorption so that the body uses its cholesterol to keep making more bile salts.
- Nicotinic acid (Niacin) decreases the production of LDL.
- HMG-CoA reductase inhibitors decrease cholesterol synthesis. These medications include Lovastatin, Pravastatin, Simvastatin and Atorvastatin.
- Fibric acid derivatives such as Gemfibrozil increase HDL and decrease triglyceride levels.
Obesity
Obesity is defined as being 20% over maximum desirable weight for your height. The Body Mass Index (BMI) is the most widely used formula for determining obesity: (weight/height2). A BMI of 20-25 is considered good, over 27 is considered overweight, and over 30 is considered obese. To calculate your BMI, visit this Web site. Obesity increases the risk of heart disease by increasing other risk factors such as high blood pressure, diabetes, and lowering HDL (good cholesterol).
Diabetes Mellitus
Diabetes Mellitus increases the risk of heart disease because it elevates cholesterol levels and increases atherosclerosis. Furthermore, people with diabetes are often overweight thereby exacerbating their diabetes and increasing the risk of heart disease. There are two types of Diabetes, Type I (insulin dependent) and Type II (non-insulin dependent). In Type I diabetes, very little or no insulin is produced by the pancreas so this condition is treated with insulin. In Type II diabetes, insulin is still being produced by the pancreas but the body is resistant to it. Type II diabetes can be treated by weight loss, a modified diet and an exercise regimen. If these methods are unsuccessful, medications called Oral Hypoglycemics are used. By increasing the secretion of insulin by the pancreas, these medications usually work. However, if these fail, insulin may be necessary.
Stress
High levels of stress and having what is known as a "Type A personality" may be risk factors for heart disease. Stress can cause your heart to work harder by increasing your blood pressure and pulse. Learning to calm down, slow down, and relax can help ease the effects of stress. It can also be beneficial to avoid caffeine and nicotine, and incorporate some type of exercise regimen into your daily routine.
Sedentary Lifestyle
Having a sedentary lifestyle leads to being overweight which can then lead to diabetes and elevated blood pressure -- both are risk factors for CAD. Exercise may lower LDL and increase HDL. It also strengthens the heart and increases its efficiency as well as the efficiency of the body's use of oxygen. People who exercise generally have a slower pulse and this puts less strain on the heart.
In the following sections, we'll look closely at angina and heart attack, two conditions that can result from atherosclerosis.