It seems that whenever there's an outbreak of a virus or disease, there's also an outbreak of conspiracy theories, false cures and, occasionally, dangerous information. A lot of online talk about the Ebola virus — particularly around the 2014 outbreak — has included some interesting chatter about blood types — and particularly those with Rh-negative blood. The story is that people with the Rh-negative blood type have a natural immunity to viruses, including Ebola. We've delved into this theory to separate fact from fiction and find out how it evolved.
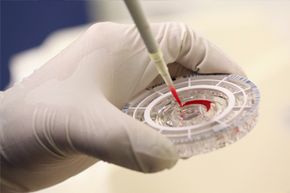
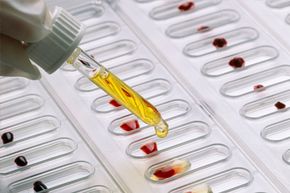
First, let's talk facts, starting with a refresher course on blood types. Everyone has different "markers" in their red blood cells (also called antigens). They identify our blood cells to our own body and help our body recognize an invader. Humans can have one of four main blood groups, and each type has its own marker: A, B, AB and O.
Advertisement
On top of these four blood types, some people have an extra marker, called the "Rh factor." Rh is an abbreviation for "rhesus." If you have the Rh marker, you are Rh-positive. Rh-positive blood is much more common than Rh-negative blood. Around 85 percent of Caucasians are Rh-positive, with those of African descent, Asians and Native Americans having an even higher percentage [source: Penn State Hershey]. If you don't have the marker, you are "Rh-negative." This percentage of people is much lower.
However, having any sort of genetic marker in your blood doesn't really make much of a difference, health-wise. The only time the Rh factor really comes into play is during a woman's pregnancy. If you're Rh-positive and the father is Rh-negative, there's no cause for concern. If both you and the father are Rh-negative, there's no reason to worry either.
However, if you're Rh-negative and the father is Rh-positive, you and your fetus can experience blood incompatibility [source: Penn State Hershey]. If Rh-positive blood (the fetal blood) gets into your system, your blood can start producing antibodies that could attack the baby's red blood cells, causing anything from anemia to more serious complications. In the past, this used to be a dangerous risk, but now the mother can take a vaccine to prevent blood cells from attacking the fetus.
We don't really know why people have this extra antigen any more than we know why some people have Type A blood and some people have Type B blood. Geneticist Khameeka Kitt explains that most differences are simply caused by run-of-the-mill DNA mutations occurring over the course of evolution. She mentions a theory, though, that Rh-negative individuals appear to be more resistant to the Toxoplasma parasite. However, it's just a theory for now.
The bottom line is that we have a lot more to learn and understand about the Rh factor, and the words "more resistant" do not mean "immune." However, a handful of people think they have the answer about the Rh factor, and that answer is, well, really "out there."
Advertisement