An infection occurs when organisms with the potential to cause disease enter the body. They can cause swelling, redness, pain and a heightened body temperature.
Usually when you talk about infections, you mean something like an ear infection, or maybe a cut that got infected — basically, some germs got into a squishy part of the body. It makes sense; our bodies are made up mostly of soft tissues, organs and blood, so usually that's where we get infections. However, your squishy bits aren't the only places that can wind up infected. Although you may not hear about it much, you can also get an infection inside your bones.
Advertisement
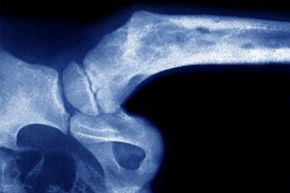
Bone infections (or osteomyelitis) affect about two in every 10,000 people, and they're twice as common among men [sources: Cleveland Clinic, PDRhealth]. Osteomyelitis can happen to any bone in the body. In adults, it typically occurs in the spinal or pelvis areas. Whereas adults are more likely to have chronic osteomyelitis, children tend to get acute infections, usually in the long-bone areas such as the legs or arms that can impair bone growth.
So, how do you contract a bone infection? It can travel through the bloodstream, spread from nearby tissue, or settle into the bone itself.
Bacteria that enter the body can travel all over and settle in just about anywhere. For example, if you have damaged heart valves, bacteria might flock there because they know the heart is too weak to fight them off [source: LifeBridge Health]. Think of your body as an army and the bacteria as the opposing troops; they look for the weak spots and exploit them.
Your bones are built to protect themselves against infection, but sometimes bacteria get in anyway. If a contaminated object penetrates your bone (think a nail going through your shoe or a deep dog bite), infection can set in. People who suffer severe broken bones — where the bone penetrates the skin — are also vulnerable to bacteria entering the bone directly. Bacteria can enter the joints and slowly eat away at them, causing arthritis or permanent joint damage. Very rarely, if a bone infection continuously drains through a sinus tract for a long period of time, cancer can develop [source: LifeBridge Health].
People with diabetes, sickle cell anemia or poor circulation may have damaged blood vessels that allow bacteria to overpower infection-fighting cells. People with poorly controlled diabetes can develop serious skin infections — especially in the feet — that make them vulnerable to osteomyelitis. Among children, a common cause of osteomyelitis is an existing infection making its way through the bloodstream to the growth plates, or soft ends of the bones and joints — a condition known as hematogenous osteomyelitis [source: PDRhealth]. Other people susceptible to bone infections include those with AIDS and HIV, sickle cell anemia, rheumatoid arthritis and suppressed immune systems.
A bone infection can be pretty serious. The main culprit when it comes to bone infections is the bacteria Staphylococcus aureus, also called staph, but other types of bacteria and even fungal infections can be the bad guys, too.
Symptoms of a bone infection include:
- Fever
- Redness and swelling at the site
- Bone pain
- Nausea
- Pus at infection site
- Increased white blood cell count, signifying infection
As horrible as all of this sounds, there are ways you can reduce your risk.
Advertisement