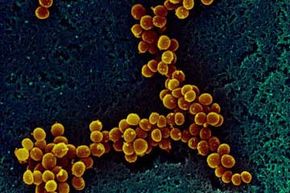
If you've ever been hospitalized, then chances are you've noticed many of the precautions taken to prevent infections in patients. One of the most serious known infections to cause trouble in hospitals is the staph infection. Caused by Staphylococcus bacteria, these infections can invade your skin, lungs, urinary tract, heart and bloodstream. To fully understand the effects of staph infections on the body today, it's best to look back on how they have evolved over the past few centuries.
In 1881, Scottish surgeon Sir Alexander Ogston discovered and named the primary cause of wound infection "Staphylococcus." Until this time, no one knew what exactly was causing wounds to become infected. In 1928, the bacteria-fighting medication penicillin was discovered, and in 1941, it was used to cure a British policeman who had a strain of Staphylococcus. Penicillin proved helpful for curing staph infections for a few years, but its widespread use caused the staph bacteria to mutate and become resistant to the treatment. Fortunately, in 1959, a new cure was found in methicillin, an antibiotic related to penicillin. However, by 1961, the bacteria had mutated again to resist it, creating a new strain called methicillin-resistant Staphylococcus aureus, or MRSA. The introduction of MRSA led to a change in infection control practices, but it still remains a threat [source: Orent].
Advertisement
Because of its resiliency, MRSA is often considered the most frightening type of staph infection, but it's certainly not the only kind. Staph bacteria can live on people as well as inanimate objects without anyone being the wiser, and many people can carry the bacteria without ever having an infection. There are more than 30 types of staph bacteria, causing a wide variety of symptoms we'll look at more closely later. The most common type is Staphylococcus aureus, which can cause infections like cellulitis, impetigo and boils on the skin. It can also cause non-skin-related illnesses such as toxic shock syndrome and food poisoning. If not properly treated, staph can cause serious illness and can result in death.
Up until the 1990s, staph was most commonly found in hospitals [source: Borlaug]. However, as we'll see in the next section, it has begun to spread outside medical facilities.
Advertisement