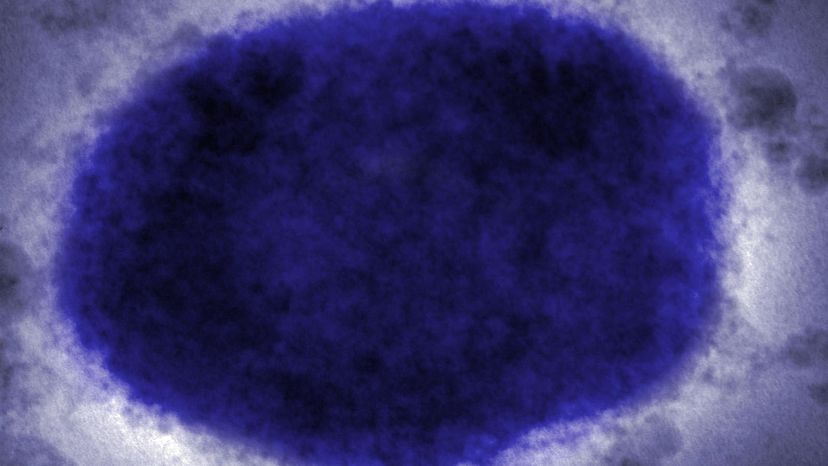
Contrary to its name, monkeypox is not usually spread by monkeys; it was given the moniker after it was first isolated from a monkey colony in 1958. The virus is typically spread by small rodents such as dormice, rats, and tree and rope squirrels. Scientists still haven't pinned down which species is the natural reservoir for the disease, though some kind of rodent seems likely.
In 1970, the first case of monkeypox in humans was recorded in the Democratic Republic of the Congo. To this day, the DRC and other Central and West African countries, including Nigeria, see the vast majority of monkeypox outbreaks. Cases usually crop up in heavily forested, rural areas. "These are populations that are routinely hunting wild animals or have close contact with wild animals in the forest," McCollum says.
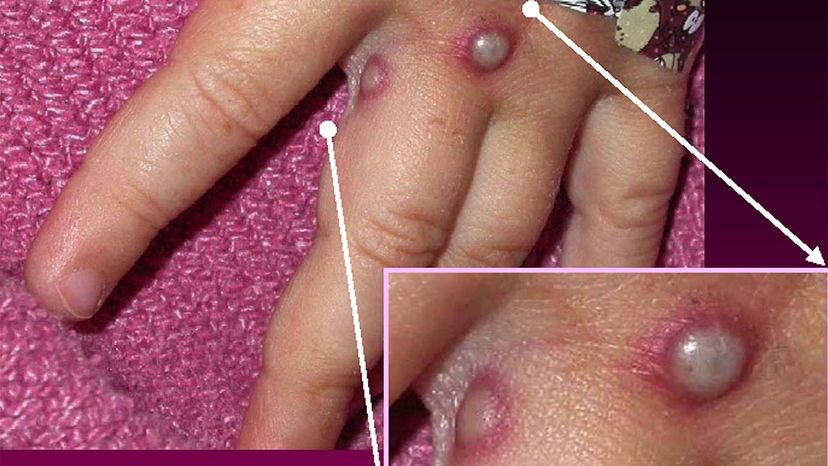
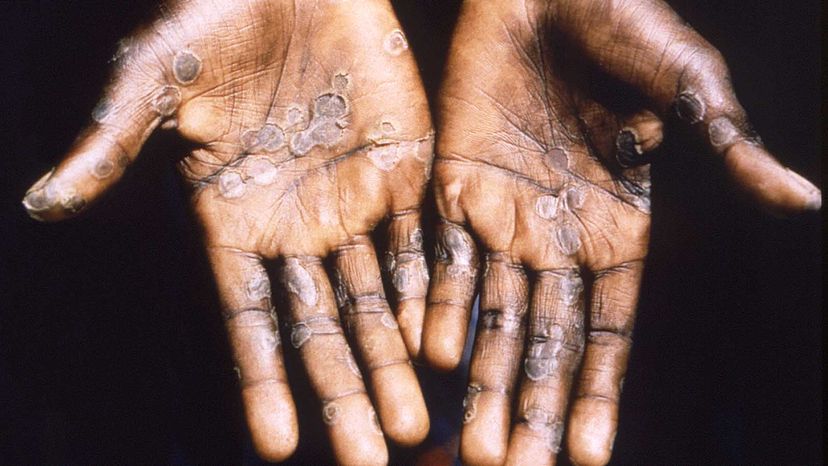
Once a human contracts monkeypox, they can pass it to other humans via respiratory droplets or contact with skin lesions. It is much less contagious than COVID-19 or other respiratory viruses when spread through the air, but it can linger on surfaces. Typically, close family members or caregivers of people with monkeypox are at the highest risk of becoming infected. Animal-to-human transmission also can occur when someone is bitten or scratched by an infected animal or if they eat infected bush meat.
So how likely is monkeypox to become a pandemic? In short, it's not likely, but we should continue to be cautious.
Like the patient in Massachusetts, seven of the eight confirmed cases in the U.K. had not traveled to Africa, and had no contact with the one patient who was known to have traveled to Nigeria, the U.K. Health Security Agency (UKHSA) said. That suggests they caught the virus in England. The UKHSA also said more than half of the cases in London are in gay or bisexual men. It is urging men who are gay and bisexual to be aware of any unusual rashes or lesions and to contact a sexual health service immediately.
"This [outbreak] is rare and unusual," Dr. Susan Hopkins, UKHSA chief medical adviser, said in a statement Monday, May 16. "UKHSA is rapidly investigating the source of these infections because the evidence suggests that there may be transmission of the monkeypox virus in the community, spread by close contact."
"Many of these global reports of monkeypox cases are occurring within sexual networks," Inger Damon, M.D., Ph.D., said in a statement. Damon is the director of the CDC's division of High-Consequence Pathogens and Pathology and a poxvirus expert with more than 20 years' experience. "However, health care providers should be alert to any rash that has features typical of monkeypox. We're asking the public to contact their health care provider if they have a new rash and are concerned about monkeypox."