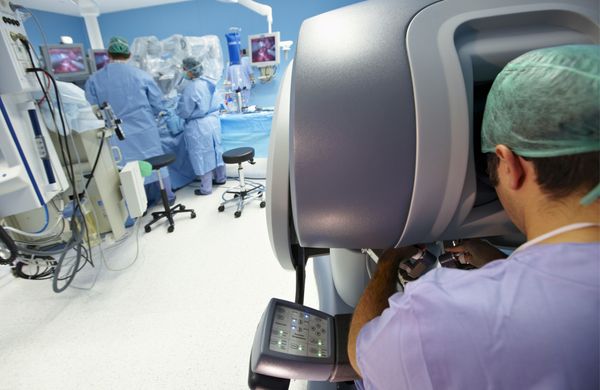
The term "robotic surgery" may conjure up the image of an android such as C-3P0 from "Star Wars" clad in a gown and mask. But surgical robots are just mechanical arms to which tiny tools, sensors and cameras can be attached. A human doctor controls the robotic arm using a computer and a screen that allows him or her to view enlarged 3-D images of the body.
In some ways, robotic surgery is similar to minimally invasive surgery, in that it allows an operation to be performed through a smaller incision than conventional open surgery. But it's even less invasive, because a robotic arm can make smaller, more precise movements than the surgeon who is directing it, minimizing damage to tissue [source: MedlinePlus].
Advertisement
The history of robotic surgery dates back to 1985, when a neurosurgeon used a robot called the Puma 560 to perform delicate brain biopsies with greater precision than a human hand could [source: Lanfranco et al.]. Since then, robotic surgery has been used for a wide range of surgical procedures, from coronary artery bypasses and tubal ligations to kidney transplants and prostate cancer surgery [source: MedlinePlus]. Since the late 1990s, doctors have performed more than 1.5 million operations using the da Vinci robotic system, a $1 million device with four robotic arms that allows surgeons to control up to 50 different instruments [source: Glass and Knight].
But the growth in robotic surgery also has exposed its limitations. Some critics note that robotic arms can't feel human tissue in the way that a surgeon's actual hand can, and that sensors designed to provide tactile feedback still have difficulty compensating for vibration and other distorting effects [sources: Glass and Knight, Kreml]. Hopefully, improvements in sensor technology and software will conquer that problem.
Other technological advances could enable robots to truly revolutionize surgery in the future. Researchers envision merging robotics with artificial intelligence, virtual reality and gadgetry that allows machines to be controlled remotely by brain waves. The operating room of the future may be a VR simulation of the inside of a patient's body, in which doctors can see through tissue and control surgical robots with their minds, while working alongside other autonomous robotic assistants. Surgeons will even be able to augment the 3-D environment with data from other scans or medical tests, so that they'll see the cancerous tissue inside a kidney as, say, bright green [source: Shubber].
Researchers are also developing tiny surgical robots -- nanobots -- that may someday roam inside the body on their own. Others envision robots with innovative designs, such as a flexible snake robot that would crawl inside a surgical incision and slither into places where human hands or conventional tools couldn't reach [source: Begos]. We've come a long way from bloodletting, but there will always be room for innovation.
Advertisement