If teachers still showed hygiene films in health class, millions of pubescent students would be advised to bathe frequently as a way to battle increasingly common bouts with body odor. Turns out, there's a physiological reason for our propensity for stinkiness in the teenage years and beyond -- and it all has to do with apocrine sweat glands.
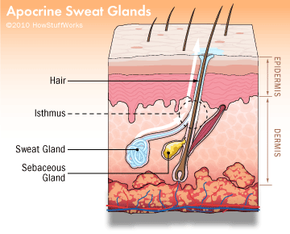
That's because apocrine sweat glands are found in the places where we have the most hair follicles (the scalp, armpits and groin) and they produce plentiful meals for bacteria. In fact, apocrine glands are one of two types of sweat glands found on mammals. The other type, eccrine glands, is designed to secrete odorless perspiration laced with salt and electrolytes. However, apocrine sweat glands release a fat-infused liquid that, when pushed to the surface of the skin, is eaten by bacteria. And that's where the odor comes into play [source: Mayo Clinic].
Advertisement
So, other than staying fresh with some good ol' soap and water, what else do we need know about apocrine sweat glands? Plenty. These glands can be the sites of some pretty serious medical conditions, at least one of which is on the rise. We'll sort out the inner workings of apocrine sweat glands, next.