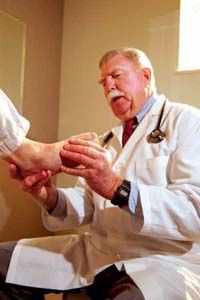
The Diabetic Foot
Even though it looks much the same as any other foot, the diabetic foot requires special attention. Why? Nerve damage is common with diabetes, especially in the lower extremities. Blood vessels are damaged as a result of the disease and circulation is decreased. When this happens, feet and legs tend to be cold and sores heal slowly, in some cases taking years to heal. This can easily lead to infection. Nerve damage can also decrease your ability to feel sensations in your feet, such as pain, heat, and cold. That means you may not notice a foot injury until you have a major infection.
A common complaint from many people is, "My feet are killing me!" For a person with diabetes, that statement could be all too true. Loss of nerve function, especially on the soles of the feet, can reduce feeling and mask a sore or injury on the foot that, if left unattended, can turn into an ulcer or gangrene.
Neuropathy, damage to the nerves, is a common problem for people with diabetes. It occurs most often in the feet and legs, and its signs include recurring burning, pain, or numbness. In addition to being painful, neuropathy can be harmful because if it causes a loss of feeling in the foot, even a minor foot injury may go undiscovered. In extreme cases, this can lead to serious infection, gangrene, or even amputation of the limb. Because of this, people with diabetes must be meticulous in caring for their feet.
Moderate exercise, such as walking, cycling, or swimming, are best for people with diabetes. Because people with diabetes have to take some extra precautions while exercising, you will need to work with your health-care provider to design an exercise program that is right for you. For example, since exercise lowers blood glucose, you will need to learn how to maintain the correct balance of food, exercise, and medication to prevent your blood glucose levels from dropping too low.
Your doctor may recommend that you avoid intense, high-impact activities such as running because of the potential for foot injury. Also, intense exercise could endanger tiny blood vessels in the eyes that are already weakened by diabetes (all that glucose in the blood can damage fragile vessels as well as nerves), potentially leading to rupture, vision problems, and even blindness. Overall, however, the benefits of exercise far outweigh the risks, and if you work with your doctor to create an exercise plan, you should be fine. Keep in mind that if you are over 40 years old, you will need to undergo a general medical examination, including a cardiovascular screening and exercise test, before proceeding with your exercise program.
Once your doctor gives the go-ahead, you need to set realistic goals in order to avoid too-high or too-low blood glucose levels. Begin with small goals, such as exercising for five minutes three days a week, and work up gradually to exercising for 30 minutes a day most days of the week.
It's important to take excellent care of your feet. Here are some tips on how to do that:
Look them over. Give your feet a thorough going-over every night to make sure that you haven't developed a sore, blister, cut, scrape, or any other tiny problem that could blow up into big trouble. If your vision isn't good or you have trouble reaching your feet, have someone check your feet for you.
Wash, rinse, and dry. A clean foot is a healthy foot, with a much lower susceptibility to infection. And clean feet feel better, too. Don't forget to clean and dry between the toes.
Avoid bathroom surgery. Under normal circumstances, there is little danger from using a pumice stone to reduce a corn or callus. But for a person with diabetes, such a practice might lead to a little irritation, then a sore, then infection, and finally, a major ulcer. Likewise, caustic agents for removing corns and calluses can easily cause a serious chemical burn on your skin. Never use them. If you develop a corn, callus, wart, or other foot problem, see a podiatrist.
Take care of the little things. Any time a cut, sore, burn, scratch, or other minor injury appears on your foot, attend to it immediately by washing it and covering it with protective sterile dressing. If you use adhesive tape, remove it carefully because it can weaken the skin when you pull it off. Consider using paper or cloth tape instead. If the sore is not healing or if you notice signs of infection, such as redness, red streaks, warmth, swelling, pain, or drainage, see a podiatrist.
Choose shoes with care. Select shoes that fit both feet well and won't cause blisters or sores on your feet. Specialty diabetic shoes are available.
Have your feet checked. Be sure your doctor examines your feet during your regular check-ups; taking your shoes and socks off as soon as you get in the exam room may serve as a reminder for you both. Or, find a podiatrist experienced in treating diabetic feet and together set up a schedule for regular foot check-ups, perhaps coinciding with nail trimming if you are unable to take care of this task yourself.
Go easy on the heat. Don't be tempted to warm your cold feet with a heating pad or hot water bottle. If you have neuropathy, you may burn yourself without even feeling it. Instead, wear warm socks, or indulge yourself in a gentle foot massage. Make sure that after the massage, you clean away any remaining oil from between your toes. A mild solution of vinegar and water will do it.
Expect dry skin. The nerves that control sweating in your feet may no longer work. So, after a bath, dry your feet and coat them with a thin layer of moisturizer. DO NOT use oils or creams between your toes. DO NOT soak your feet. The more you do, the more you put yourself at risk for infection. Moisture there can cause an infection, such as athlete's foot.
Diabetes is a serious health risk that plagues millions of Americans. However, the home remedies and strategies in this article can help you manage the disease and live a healthy and rewarding life.
ABOUT THE AUTHORS:
Linnea Lundgren has more than 12 years experience researching, writing, and editing for newspapers and magazines. She is the author of four books, including Living Well With Allergies.
Michele Price Mann is a freelance writer who has written for such publications as Weight Watchers and Southern Living magazines. Formerly assistant health and fitness editor at Cooking Light magazine, her professional passion is learning and writing about health.
Ivan Oransky, M.D., is the deputy editor of The Scientist (www.the-scientist.com). He is author or co-author of four books, including The Common Symptom Answer Guide (McGraw-Hill, 2004), and has written for publications including the Boston Globe, The Lancet, and USA Today. He holds appointments as a clinical assistant professor of medicine and as adjunct professor of journalism at New York University.
ABOUT THE CONSULTANTS:
David J. Hufford, Ph.D., is university professor and chair of the Medical Humanities Department at PennsylvaniaState University's College of Medicine. He also is a professor in the departments of Neural and Behavioral Sciences and Family and Community Medicine. Dr. Hufford serves on the editorial boards of several journals, including Alternative Therapies in Health & Medicine and Explore.
ABOUT THE EDITORIAL CONTRIBUTORS:
Timothy Gower is a freelance writer and editor whose work has appeared in many publications, including Reader's Digest, Prevention, Men's Health, Better Homes and Gardens, The New York Times, and The Los Angeles Times. The author of four books, Gower is also a contributing editor for Health magazine.
Alice Lesch Kelly is a health writer based in Boston. Her work has been published in magazines such as Shape, Fit Pregnancy, Woman's Day, Reader's Digest, Eating Well, and Health. She is the co-author of three books on women's health.
This information is solely for informational purposes. IT IS NOT INTENDED TO PROVIDE MEDICAL ADVICE. Neither the Editors of Consumer Guide (R), Publications International, Ltd., the author nor publisher take responsibility for any possible consequences from any treatment, procedure, exercise, dietary modification, action or application of medication which results from reading or following the information contained in this information. The publication of this information does not constitute the practice of medicine, and this information does not replace the advice of your physician or other health care provider. Before undertaking any course of treatment, the reader must seek the advice of their physician or other health care provider.