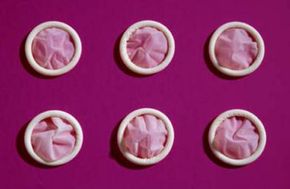
You might not want to talk about them, but infections that occur in the genital area can be dangerous. It's probably been awhile since you last had health class, but you need to shake off your embarrassment to keep your private parts working their best. In this article, you'll find:
- Preventing Chlamydia An estimated 2.8 million Americans are infected each year with the STD Chlamydia. And, according to the Centers for Disease Control and Prevention, the people who are most at risk include those with multiple sex partners and sexually active teenage girls. Learn more about Chlamydia in this section, including what steps you can take to prevent this STD.
- Preventing Genital Herpes Genital herpes is typically caused by the herpes simplex virus type 2 (HSV-2). Although this sexually transmitted disease can be treated with antiviral, suppressive medications to shorten and prevent outbreaks, there is no actual cure for genital herpes. Find out how to avoid contracting genital herpes here.
- Preventing Gonorrhea The symptoms of gonorrhea are different for men and women, although if left untreated, this STD can cause infertility in both sexes. Fortunately, most strains of this bacterial infection can be treated with antibiotics. Learn more about the common symptoms and what you can do to stay away from gonorrhea on this page.
- Preventing Human Papillomavirus The Centers for Disease Control and Prevention report that at least half of all sexually active men and women will have an Human Papillomavirus (HPV) infection at some point in their lives. That's quite a statistic! Gather all the facts about HPV, including measures you can take to defend yourself against this STD, in this section.
- Preventing Syphilis If not treated properly, the STD syphilis can ultimately be a fatal disease. There are four stages of this infection, so it's important to know what to look out for in the early stages to prevent serious problems. You should also learn how to prevent syphilis by reading the suggestions on this page.
This information is solely for informational purposes. IT IS NOT INTENDED TO PROVIDE MEDICAL ADVICE. Neither the Editors of Consumer Guide (R), Publications International, Ltd., the author nor publisher take responsibility for any possible consequences from any treatment, procedure, exercise, dietary modification, action or application of medication which results from reading or following the information contained in this information. The publication of this information does not constitute the practice of medicine, and this information does not replace the advice of your physician or other health care provider. Before undertaking any course of treatment, the reader must seek the advice of their physician or other health care provider.
Advertisement