In the past 20 years, biotechnology has become the fastest-growing area of scientific research, with new devices going into clinical trials at a breakneck pace. A bionic arm allows amputees to control movements of the prosthesis with their thoughts. A training system called BrainPort is letting people with visual and balance disorders bypass their damaged sensory organs and instead send information to their brain through the tongue. Now, a company called Second Sight has received FDA approval to begin U.S. trials of a retinal implant system that gives blind people a limited degree of vision.
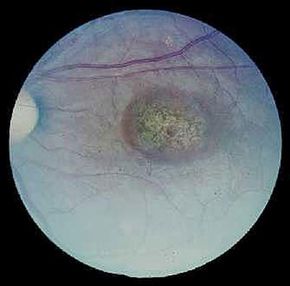
The Argus II Retinal Prosthesis System can provide sight -- the detection of light -- to people who have gone blind from degenerative eye diseases like macular degeneration and retinitis pigmentosa. Ten percent of people over the age of 55 suffer from various stages of macular degeneration. Retinitis pigmentosa is an inherited disease that affects about 1.5 million people around the globe. Both diseases damage the eyes' photoreceptors, the cells at the back of the retina that perceive light patterns and pass them on to the brain in the form of nerve impulses, where the impulse patterns are then interpreted as images. The Argus II system takes the place of these photoreceptors.
Advertisement
The second incarnation of Second Sight's retinal prosthesis consists of five main parts:
- A digital camera that's built into a pair of glasses. It captures images in real time and sends images to a microchip.
- A video-processing microchip that's built into a handheld unit. It processes images into electrical pulses representing patterns of light and dark and sends the pulses to a radio transmitter in the glasses.
- A radio transmitter that wirelessly transmits pulses to a receiver implanted above the ear or under the eye
- A radio receiver that sends pulses to the retinal implant by a hair-thin implanted wire
- A retinal implant with an array of 60 electrodes on a chip measuring 1 mm by 1 mm
On the next page, we'll look at how the whole mechanism comes together.
Advertisement