Your blood delivers essential nutrients (such as amino acids), electrolytes, antibodies, hormones, vitamins and oxygen to all the tissues throughout the body, and it carries away carbon monoxide and waste. It's not just on the menu for the undead; it keeps the human body running, and without it you couldn't survive a vampire attack or just a normal day. But it's not just ]Nosferatu and those bloodthirsty summertime mosquitoes who want to suck your blood. Every two seconds, someone in the U.S. needs blood, or a blood component. There's no substitute for the real thing -- and a single victim of a car crash could require as many as 100 pints of life-saving blood.
Your body needs real blood to function properly, and blood cells, platelets and plasma -- the basic components of human blood -- are only available from human donors. About 38 percent of American adults are eligible blood donors, but fewer than 10 percent of those who can actually donate to the blood supply -- that equals about 9.2 million people donating blood every year. [source: American Red Cross].
Advertisement
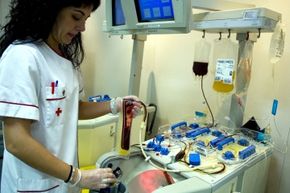
Healthy bodies are continually regenerating their own blood, which means blood donors need only wait a few weeks between donations, depending on what you're donating. While no one ever has said they want to suck your plasma, plasma's an important component of blood; the body regenerates plasma faster than it's able to make blood, which means healthy people can donate plasma as often as twice in one week as long as they get about 48 hours of recovery in between visits. Some donation centers and blood banks recommend you wait 28 days between plasma donations; for comparison, the minimum waiting time to donate blood is eight weeks [sources: Access Clinical, Carter BloodCare].
But before you can decide if you want to be a blood or plasma donor, you need to know whether or not you're eligible; while blood donations often fall short of need, not all of us make good donors.
There are a few things to keep in mind as a donor candidate. For instance, did you know if you spent three or more months in the U.K. between 1980 and 1996 you can't donate blood in the U.S.? You can't, indefinitely -- it has nothing to do with how you spent your time there and everything to do with variant CJD (vCJD) concerns (that's the human form of bovine spongiform encephalopathy, or mad cow disease).
Let's talk about who is and who isn't eligible to donate.
Advertisement