Unless you're a detective, a thief or a strangely nosy person, you wouldn't take your neighbor's trash and dump it in your kitchen, let alone consume it. On the other hand, if you were dying of scurvy, those limes they threw away after last night's margarita party might look surprisingly appetizing.
Accepting a transplant of someone else's stool, however carefully tested, might sound just as extreme, but -- thanks in part to its effectiveness in treating the intractable bug Clostridium difficile -- fecal microbiota transplantation might just be the next big thing in medicine [sources: Grady; Hudson; Mayo Clinic].
Advertisement
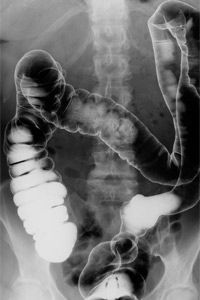
C. difficile, an emerging epidemic in hospitals and nursing homes, primarily affects older patients during long stays in care facilities. Like opportunistic weeds, the bacteria move into areas of the gut decimated by the very antibiotics intended to oust infections (antibiotics don't distinguish bacterial friend from foe). Once in the gut, C. difficile cranks out toxins that damage the intestinal lining, causing symptoms ranging from diarrhea to life-threatening colon inflammation. To make matters worse, C. difficile has grown increasingly virulent and antibiotic-resistant in recent years [sources: Grady; Hudson; Mayo Clinic].
Sending bacteria to fight bacteria makes good sense. Far from being a mere batch of bugs, many bacteria and other microbes are not only our friends, they are part of us. Our bodies contain nine to 10 times as many microbial cells as human ones; we each play host to 100 trillion bacteria. It's all part of a microbiome, an ecosystem of microbial communities that perform all kinds of useful work, from enabling digestion to aiding our immune systems [sources: Khoruts; Zimmer; Zimmer].
The recognition of microbial contributions to health has given rise to the growing field of medical ecology, which approaches the body's microbiome as a garden to be nurtured and, if necessary, weeded. Fecal transplantation extends this philosophy to "organically mulching" the gut garden: Stool from a healthy donor contains beneficial gut microorganisms, aka flora, 60-80 percent of which will take up residence in the recipient's gut, replacing those destroyed by antibiotics and infections, and overthrowing harmful communities like C. difficile [sources: Borody; Hudson].
Driving the need for such novel techniques are the ever-increasing numbers of people, particularly the elderly, who die each year from gastrointestinal infections. In the U.S. such deaths more than doubled from 1999 to 2007, rising from 7,000 to more than 17,000 a year [source: CDC]. Eighty-three percent of those fatalities occurred among patients over 65, two-thirds of whom died from C. difficile infections [source: CDC].
Fecal microbiota transplantation might sound outlandish or even a bit disgusting, but it restocks the body with some of the many microbes it needs to recover, live and thrive.
Advertisement