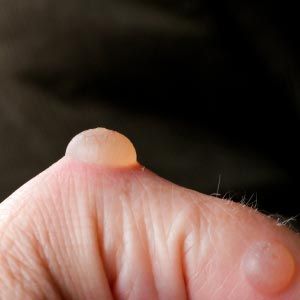
If you notice a spot growing on your newborn son or daughter, your first reaction is probably alarm. But if the lesion is small and red, there's probably no need to worry. You should definitely have it looked at by a doctor, but chances are it's just a hemangioma. Despite their ominous name, hemangiomas are just vascular birthmarks made from growths of extra blood vessels. They also happen to be pretty common; about one in every 50 babies develops a hemangioma [source: Greene].
Hemangiomas typically develop on the skin as flat, red lesions that grow over time, and they can be divided into two main types: capillary and cavernous [source: O'Malley]. Capillary hemangiomas, once commonly known as strawberry hemangiomas and sometimes called superficial hemangiomas, appear as raised, red growths on the skin's surface. Cavernous hemangiomas are sometimes called deep hemangiomas because they develop beneath the skin and bulge out, turning the skin above them a shade of purple. Growths that are both capillary and cavernous are called compound hemangiomas, and they tend to grow large [source: American Osteopathic College of Dermatology].
Advertisement
Unlike other birthmarks, hemangiomas aren't usually permanent. They typically appear soon after the baby is born and grow larger before beginning a very slow process of shrinking [source: Mayo Clinic]. Most of them disappear on their own, but sometimes it can take as much as 10 years for this to happen. For the most part, hemangiomas are harmless and painless, but it's important to keep an eye on them because they can cause problems if they develop near an eye or an ear. There are also rare cases in which hemangiomas can become life-threatening, so if your infant develops one, you'll want to have a doctor look at it so it can be treated [source: Cincinnati Children's].
Keep reading to find out the cause behind these common birthmarks.
Advertisement