It would be so much easier for millions of people if replacing teeth was simply a matter of finding new ones and popping them in place. Smile -- you're done. Of course it's a bit more involved than that, whether you opt for traditional dentures or dental implants.
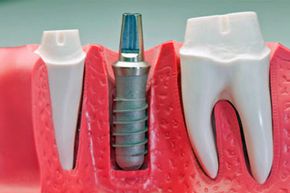
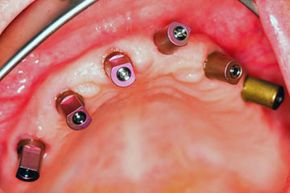
Dentures and bridges are the most common and affordable option for tooth replacement, but implants are considered to be as close to natural teeth as you can get [source: JADA]. (The term "dental implants" actually applies to the replacement tooth roots that provide the foundation for the permanent or removable teeth; but it's used interchangeably for the teeth themselves, as well.) Most implants are made from titanium or titanium alloys, which are very strong and lightweight metals; the teeth are made from porcelains and other composite materials designed to look like and match real teeth.
Advertisement
Think of getting dental implants like installing a fence post. The first step is to dig a hole into the ground so a supporting beam can be lowered in. Sometimes the post is secured with cement that needs to dry, and often it is packed in with dirt that gives it the foundation it needs to stand straight and tall to support the fence.
Building a good tooth implant is similar in that a trained surgeon makes a hole in the jaw bone and, after the implant is secured, the gum tissue and bone need to grow around it to give it the strength to hold the post that will in turn support the restored crown between other teeth. It's less of a cosmetic endeavor and more of a building process.
Many people are good candidates for dental implants, but a dentist, oral and maxillofacial surgeon and a periodontist often work together to ensure that an individual has the gum health and bone structure needed for a successful and long-lasting implant. This dental and surgical team will complete thorough exams and X-rays and will set a treatment plan. Implant surgery isn't accomplished in a single visit or even a couple of visits but progresses over many months [source: Mayo Clinic].
But why go under the knife at all when other options exist? And even if you are a candidate, can your wallet handle it? We'll look at the real differences in artificial tooth options, next.
Advertisement