Guess how many American adults have had tooth decay in their permanent teeth. One third? One half? In fact, 92 percent of Americans ages 20 to 64 have had a cavity as an adult, and just shy of a quarter of that age group have untreated tooth decay [source: NIDCR].
Tooth decay is, undeniably, a common problem. While surface decay can usually be treated with a filling, a tooth with deep decay -- or one that has been severely injured by accident or the trauma of recurrent dental work -- may become unhealthy, inflamed or infected. Left untreated, an infection may spread to the surrounding tissue and an abscess may form.
Advertisement
While there was a time when there was no other choice than to pull a dying tooth, dentists today try to help patients keep their natural teeth for as long as possible. One of the most common dental procedures is intended to give a tooth a second chance by treating the inflammation and infection from the inside: the root canal procedure. During a root canal procedure, decay is removed, the inside of the tooth is cleaned and filled, and the outside of the tooth is sealed and capped. Before we can really understand how a root canal is performed and why, let's first get comfortable with a few basics of a tooth's anatomy.
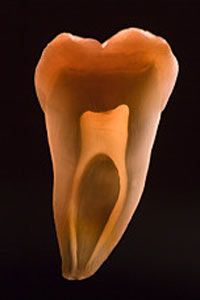
The crown of the tooth is the part that you see inside your mouth. The root of the tooth is below the gumline. The pulp is the innermost part of a tooth. It's found in the pulp chamber inside the crown of the tooth as well as in the root canal that extends from the tip of the tooth into the pulp chamber. The pulp is made up of nerves, blood vessels and connective tissues -- it's the living part of the tooth.
Root canal procedures save teeth. There are more than 15 million root canal procedures performed every year in the United States, and while your dentist is trained and capable of performing a root canal, some patients choose to have an endodontist perform the procedure [source: American Association of Endodontists]. An endodontist is a dentist who specializes in treating the inside of teeth.
To determine whether or not root therapy is needed, the dentist will first assess the patient's symptoms. Tooth ache or pain, tooth darkening or discoloration, a tooth that has developed a prolonged increase in hot/cold sensitivity and pain, or tenderness when a tooth is touched or while chewing (although some people report little to no pain) are all signs the nerve may be damaged.
While a root canal is tailored to the patient's specific dental health needs, we'll cover the basics common in every root canal procedure. Even if there is no associated pain, an unhealthy tooth needs to be treated -- while an inflamed pulp may sometimes heal on its own, an infected pulp can die without treatment, toothache or not. Let's look at what root canal treatment involves, from diagnosis to done, beginning with measuring and cleaning the inside of the tooth.
Advertisement