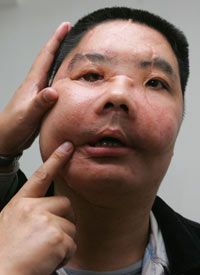
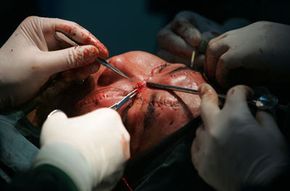
One big question everyone asks is: Will the face transplant recipient look exactly like the donor? The answer is no. Your looks are not defined solely by your skin -- the underlying bone structure also is an important factor. After the procedure, the patient will actually look like a combination of him- or herself and the donor.
Any type of surgery comes with risks, and particularly one that is as complicated as the face transplant. As with any other surgical procedure, the main risks are excess bleeding and infection. Also, a blood clot can form in one of the reattached blood vessels, blocking the blood supply to the new face and killing the tissue.
Because the face is coming from another person, rejection is always a worry, even if the tissue types closely match. The drugs used to prevent rejection come with their own risks because they suppress the immune system and lower its ability to fight off infection. People who take immunosuppressive drugs are more likely to develop diabetes, kidney disease, infections and cancer.
Patients have to endure these potential side effects and take their medicines religiously in order for the surgery to be successful. They also need to follow all of their doctors' recommendations. One hand transplant patient had to have the appendage removed when he stopped taking his anti-rejection medications. Isabelle Dinoire ignored her doctors' advice to stop smoking, which could affect the circulation to her new face [source: New York Times].
In addition to the many potential physical complications of having a face transplant, there are a number of psychological issues. Having someone else's face in place of your own is understandably traumatic, and people who undergo this operation may need counseling to regain some normalcy in their lives.
All three of the partial face transplants performed so far have been successful, but there is still a high possibility that future surgeries will fail. If that happens, doctors have one of three options: They can remove the face and perform another transplant from a new donor, resurface the face with artificial skin or cover the space with grafts of real skin.
The Controversies
Although the technology to perform face transplants has been around for many years, doctors didn't attempt the procedures until recently, mainly because of ethical concerns. The first concern is over the donor, whose family must be willing to turn off life-support machines while the person is still technically alive. Other ethicists are concerned about patients assuming the risks of major surgery when their lives are not technically in danger. Might there come a day, some have speculated, when the ultrarich will opt for face transplants simply to look prettier or younger?
In 2003, the Royal College of Surgeons in the United Kingdom issued a paper in which it warned doctors not to perform face transplants until they knew more about the risks and ethical implications of doing such a surgery. A year later, the French National Ethics Advisory Committee issued its own warning against performing the procedure. Yet despite the concerns, in just a few years doctors started performing partial face transplants -- and began gearing up to do a full face transplant. How the technology, and the debate, evolves will become clearer in the coming years.
For more information about face transplants, check out the links on the next page.