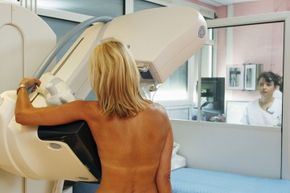
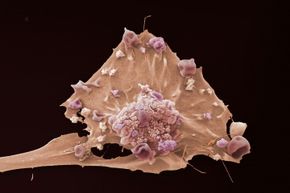
Just about one American woman out of eight -- that's as many as 12 percent -- will be diagnosed with an invasive breast cancer in her lifetime (and guys, you're not in luck: For a man that risk is much lower, but there is still a risk -- about one American male out of 1,000 will develop breast cancer in his lifetime) [source: BreastCancer.org].
Roughly 211,700 women were diagnosed with breast cancer in 2009 alone, and 40,676 women died from a metastization of the disease that same year, according to U.S. Cancer Statistics (USCS) [source: CDC]. Some people have a higher risk for developing breast cancer than others, and those factors include your age and medical history (including: reproductive history, menstruation history, breast density, history of any benign breast disease such as breast calcifications, hormone therapy use, exposure to radiation and other variables such as your level of physical activity, your diet and how much alcohol you drink). Faulty genes also increase your risk of developing breast cancer and how early it develops. Since the late 1990s, genetic testing and counseling has been available for patients who want to know if they are predisposed to developing breast cancer because of their family history. It's estimated that if you're a woman with a BRCA1 (that's breast cancer 1, early onset gene) or BRCA2 (breast cancer 2, early onset gene) mutation, you're five times more likely to develop breast cancer during your lifetime compared to a woman with a normally functioning gene [source: National Cancer Institute]. One in 10 male breast cancers are associated with the BRCA1 mutation [source: BreastCancer.org].
Advertisement
Positive results from genetic testing may trigger many patients to consider risk-reducing measures, and some insurance companies consider preventive mastectomies to be medically necessary for high-risk women, although still experimental. Each insurance company's rules, each doctor's guidelines and each patient's needs vary, but women who are at high risk for breast cancer are those who have an early-onset breast cancer diagnosis, have a strong breast cancer and ovarian cancer inheritance pattern in the family, have radiation exposure and/or have tested positive for specific genetic mutations including BRCA1 or BRCA2.
Let's talk about what the BRCA gene is.
Advertisement