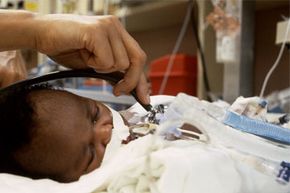
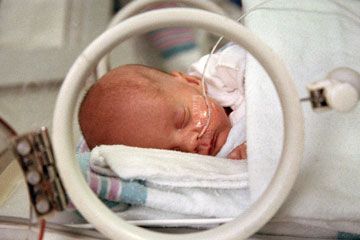
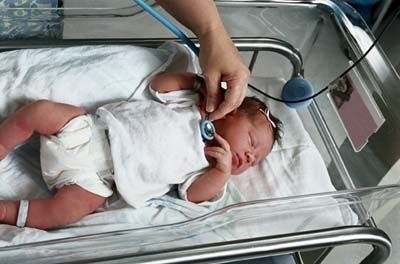
Having a baby is a life-changing event, and for most new parents, it's a happy event. However, for some families, this moment is life changing because of unforeseen complications during labor and delivery, from preterm birth to congenital malformations. Families may suddenly find themselves working with a team of neonatal specialists caring for their newborn in a neonatal intensive care unit, or NICU. NICU teams work with infants born anywhere from 23 week's gestation (micro-preemies who are born more than 4 months ahead of schedule) to full-term babies born with complications that need immediate, short or long-term attention.
We spoke with Edmund La Gamma, MD, a practicing neonatologist who is chief of the Division of Newborn Medicine in the Department of Pediatrics, professor of Pediatrics, Biochemistry & Molecular Biology at the New York Medical College and the director of the Regional Neonatal Center of the Maria Fareri Children's Hospital at Westchester Medical Center, to find out more about the NICU and just what it takes to work in one. First, Dr. La Gamma gives us an overview of how the NICU is set up.
Advertisement