In the Middle Ages, the summer solstice was a big event for Europeans. Weddings were planned for that day, and many communities held large parties with plenty of adult beverages. As a result, nine months after that day, quite a lot of babies would be born. Coincidentally, white storks returned from their migratory travels exactly nine months after the summer solstice as well, and it's believed that storks gained their reputation for bringing babies to mothers because of this scheduling sync-up [source: Adams].
Many adults may still turn to the story of the stork when they want to avoid an awkward conversation of how babies are made, but here at HowStuffWorks.com, we don't shy away from any of the tough questions. In this article, we'll explore the biology of sex -- otherwise known as human sexual reproduction. We'll examine the body's sexual organs, the biological cycles of sex and the process of fertilization. If you need a refresher on the birds and the bees, this is the article for you.
Advertisement
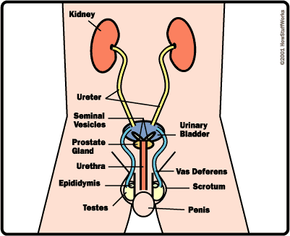
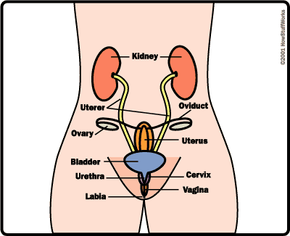
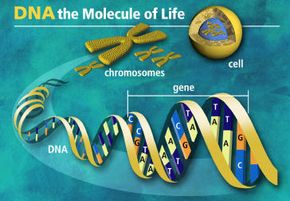
There are many reasons why people have sexual intercourse -- it improves intimacy between a couple by releasing hormones that help them bond, and studies have shown that sexual activity relieves stress, boosts immunity, reduces pain and burns calories [source: Doheny]. Those are benefits that anyone can reap from sex, no matter their gender or their sexuality. But for the subject at hand -- making a baby -- a man and a woman and their unique genetic information is required. On the next few pages, we'll discuss the reproductive systems of men and women.