Although many of us are well-educated about the various risks and rewards of pregnancy, few have any idea that the placenta, grown within a mother's own womb, can actually turn on a dime and cause allergic reaction via a rare, painful autoimmune disease.
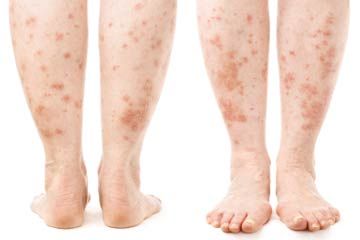
This disease, known in scientific circles as pemphigoid gestationis (PG), is characterized by painful, itchy, large blisters or welts on various body parts. In most cases, the rash begins in the abdominal area, progressing to the limbs and buttocks over time. Large, angry blisters typically appear after the patient experiences several weeks' worth of lesions and papules (swelling that resembles a pimple) [source: Huilaja et al.]. Fortunately, the genitals, face, mouth and scalp are usually spared the rash in all its blister-y glory [source: EADV]. Thank heaven for small favors, right?
Advertisement
But before you swear off pregnancy altogether, bear in mind that just a tiny percentage of pregnant women get PG. Internationally, the disease is estimated to affect one in every 2 million pregnancies, with a higher incidence in the U.S. of about one in 50,000 to 60, 000 pregnancies. Obviously, it affects only women of childbearing age, although Caucasian women are more likely to be diagnosed with it than African-Americans. Originally known as herpes gestationis (the name was changed because it turned out to have zero relation to the herpes virus), modern medicine still isn't sure why PG happens, but placental involvement is a popular theory. The prevailing idea is that normally harmless placental tissue enters the mother's bloodstream, only to be attacked by a confused immune system, as is the case with other types of autoimmune diseases. Female hormones, particularly estrogen, may aggravate the reaction, which could explain why the disease occurs during later pregnancy as estrogen levels rise [sources: Freiman, EADV]. The offensive measures taken by the immune system in error can subsequently wreak havoc on the body, in this case resulting in the allergic reaction rash. Not cool, immune system. Not cool.