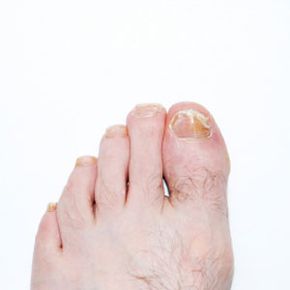
Nails are more than simple protective coverings for sensitive fingers and toes. Your nails are living, growing parts of your body, and as such, they can get sick just like the rest of your body.
Infections of the nails and the surrounding skin can result from injury, ingrown nails, split and separated nails and other more serious conditions. Infections not only cause pain, but they can also affect the way your nails grow and can impact your overall health.
Advertisement
Nails seem vastly different from the outer layer of skin known as the epidermis, but they are merely the hardening of the top layers of epidermis. On thicker-skinned parts of your body, such as your palm, the epidermis comprises five layers -- at the tips of your fingers and toes, these outermost layers of the epidermis harden into nails. These nails, made from a protein called keratin, protect the sensitive tissue underneath and make it possible to use fingers and toes for scratching and other purposes [source: O'Rahilly].
An infection occurs when foreign bodies, such as viruses, fungi and bacteria, get inside your body. Infections may seem like mild matters, but they can become serious complications for people with other medical conditions or if they go untreated and spread. Signs of infection include redness, swelling, irritation and pain. Infected tissue is also warm and tender to the touch and may produce pus [source: Breastcancer.org].
No infection should go untreated -- not even one in the smallest toenail. On the next few pages you'll learn why nail infections occur and how you can treat them.
Advertisement