It's not everyone's favorite subject -- and understandably so. For most people, developing an unsightly skin fungus may be pretty embarrassing. But such infections are actually very common. For instance, it's estimated that at any one time in the United States, at least one in five people have athlete's food, a particular type of skin fungus [source: Wallace].
Still, for many, the sight of -- or mere idea of -- a fungus living in one's skin is repulsive. But if you can distance yourself from the disgust, fungus is actually pretty fascinating. Once thought to be plants (mushrooms are still sorted among vegetables in the supermarket, after all), fungi's distinct cell walls and lack of chlorophyll distinguish them today as their own kingdom consisting of at least 80,000 species.
Advertisement
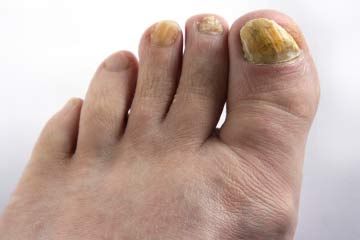
Most of the types of fungus we'll discuss are molds known as dermatophytes. These dermatophytes like to set up camp on skin because they feast on keratin, a strong, fibrous protein that makes up much of your skin (as well as nails and hair, where fungus can also thrive).
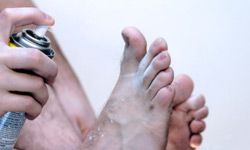
One of the most important things to keep in mind is that, besides keratin, fungus loves two things: warmth and moisture. This is why it so often holes up on sweaty feet. Skin fungus is contagious and can spread most commonly among people, but you can also get it from animals and clothes and fabrics (and even soil).
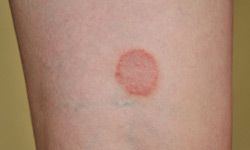
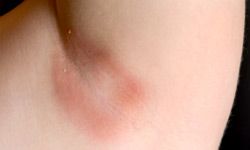
We'll go through some of the common types of skin fungus and also look at signs of getting them and how to treat them.