What do you think of when you see the word "herpes"? Painful blisters on the genital area, right? You probably know that there's no cure and that you can get it through sexual contact. Often, though, that's the extent of the average person's knowledge when it comes to herpes.
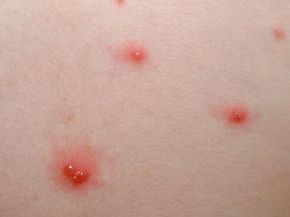
Have you ever gotten a painful, tingling fever blister on your lip? If you get cold sores, then you have herpes. If you haven't gotten cold sores, you're still not home free -- if you've had chicken pox, you're carrying a different type of herpes.
Advertisement
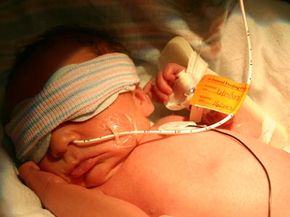
Herpes is actually a family of eight different viruses known as Herpesviridae. It's a DNA virus, which means that its genetic material is made of DNA and it replicates through RNA in the nucleus of a cell. The blisters are just the physical symptoms of the virus. If you "have" herpes, that means that you've been infected by one of these viruses at some point and it's living in your cells. Exactly where it lives depends on the type of herpes virus. Most of them are transmitted through exchange of fluids, such as semen, mucus or saliva. Some of the viruses can be passed from mother to child during pregnancy.
Most herpes viruses are cyclic. When the virus is active, an infected person experiences symptoms and associated illnesses. There's also an increased risk of passing the virus on to someone else. During the shedding stage of the cycle, the virus replicates itself, which can occur even when the virus is inactive. Even without symptoms, there is still a risk of infecting others. Many people have no idea that they have a herpes virus because they've never had any symptoms. Some types of herpes are especially prevalent; it's estimated that as many as 60 percent of adults in the United States carry the oral herpes virus and 20 percent carry the genital herpes virus [source: CDC].
Now that you know a little about herpes in general, let's start with learning about these two most well-known types.
Advertisement