Finding unexpected lumps anywhere on your body can be unnerving — and potentially scary. If the lump is an underarm cyst, the problem is generally more annoying than dangerous.
Underarm cysts — or abscesses — often form when some of your epidermal skin cells don't slough off, but instead move down under the surface of your skin and begin to grow there. This often happens as a result of a hair follicle or an oil-producing sebaceous gland within the follicle becoming damaged [source: Mayo Clinic].
Advertisement
Shaving could be to blame. But any kind of damage to the skin, such as a wound or exposure to harmful ultraviolet rays, can create the conditions that form a cyst [source: Mayo Clinic]. Once your skin is damaged or inflamed, that's when bacteria can enter. The cyst begins to form as your body tries to kill off the germs.
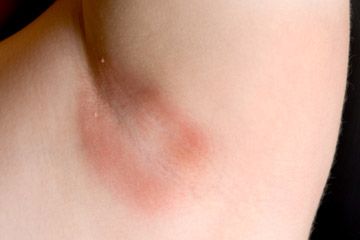
Underarm cysts are typically easy to see and feel. They're usually pinkish to red in color and are small sacs under the skin caused by the infection. They're filled with pus and bacteria and may look similar to a pimple. Unless it's infected, a cyst should be painless. They tend to be small — not much larger than 2 inches (5 centimeters) across.
However, keep in mind not all underarm lumps will be cysts. You could have a swollen or irritated lymph node (gland that helps your body fight infection). You can determine the likelihood of it being a cyst by squeezing it between your thumb and forefinger. If its wiggles back and forth easily it's probably a cyst. Another good indicator that the growth is a cyst is if you've recently injured the skin near the bump. Acne, shaving and even antiperspirants can also irritate the underarm skin and cause cysts. But the only sure way to diagnose a lump under your arm is to have your doctor examine it.
Self-treating an Underarm Cyst
Good hygiene and washing regularly are great ways to care for your skin. Unfortunately, they don't always prevent underarm cysts. If the cyst is not causing any pain or discomfort, it can be left alone. However, if you are worried it is more than a cyst, or if the cyst ruptures or becomes infected, inflamed or painful, then treatment options — described below — are available.
1. Leave It Be.
Since most cysts are usually not harmful or painful, first and quite simply, don't treat it at all. It may go away on its own [source: WebMD]. And while you might be tempted to pop it like a pimple, don't. That can damage your skin and could lead to even more infection. Plus, it doesn't guarantee that the cyst won't return.
2. Apply a Warm Compress.
A good treatment option is to apply a warm, moist towel (or flax seed heating pad) to the cyst, which could help clear it up [source: MedlinePlus: Sebaceous]. If this does encourage the cyst to drain, cover it with a bandage.
3. See Your Doctor.
If the cyst begins to become painful or is infected, you should see your doctor for treatment. If the cyst is inflamed, your doctor can inject it with steroids to reduce the swelling before treating it further.
4. Have it Drained.
If it's necessary, your doctor may choose to drain the cyst. This, however, leaves the cyst intact, allowing the possibility of it returning [source: American Academy of Family Physicians].
5. Remove the Cyst.
In a worst-case-scenario, you can have the cyst completely removed. Your doctor can do an excision where he or she not only drains the pus, but also removes the inner sac — the lining of the cyst wall — so it doesn't grow back. Or your doctor can use a laser to vaporize it [source: Mayo Clinic].
None of these procedures require a hospital stay; all can be performed in your doctor's office. At most, they will require local anesthesia — and possibly a few stitches.
Advertisement