During World War I, wounded soldiers could lie unattended for days in the no-man's-land between trenches. If they lived, they'd sometimes return to their lines with gashes and cuts crawling with fly larvae. It must have seemed to them as though matters had gone from bad to worse, but an American surgeon named William Baer noted something curious about the maggot–ridden wounds: Compared to other soldier's injuries, they looked surprisingly healthy, showing fewer signs of inflammation or infection [sources: Gabrielsen; Handwerk].
Baer had rediscovered the medical value of maggots, a quality well known to Napoleon's Army doctors and probably used by civilizations as far back as the Mayans, or by native peoples from American Indians to Australian Aborigines [sources: Gabrielsen; Soy].
Advertisement
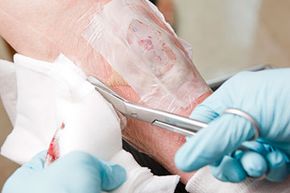
"Ick factor" aside, maggots have a lot to offer modern medicine in terms of stemming infections, speeding healing and saving money. Their forte lies in treating chronic wounds – injuries, like diabetic foot ulcers, that do not heal, or heal only slowly. In some cases, medical maggots can even help patients avoid amputation [source: Jukema et al.].
Maggots are but one example of the creatures used in biotherapy, a developing field that treats diseases using substances from living things. In this age, you might think of medical maggots as the leech's newest rival for the gag reflex award (the Food and Drug Administration has approved both creatures as medical devices). But whereas leeches suck blood — a vital quality in microsurgeries like limb reattachment, where blood buildup can kill — maggots slurp up the dead and infected tissue that hinders healing.
The FDA has also begun looking into bee-related products, a field known as apitherapy (Latin apis for bee). One example that has the medical world buzzing is bone wax, a mix of beeswax, olive oil and phenol used to stop bleeding in surgically sliced bones. Another biotherapy, bacteriophagetherapy, uses bacteria-eating viruses in place of antibiotics. Like maggot therapy, this Soviet medical technique grows more appealing as antibiotic-resistant bacteria force doctors to seek other ways to kibosh harmful microbes [source: Reardon].
Not all biotherapies are created equal, however. While some go through rigorous vetting as medical technologies, others remain little more than loose homeopathic tonics backed up by, at best, hearsay.
In other words, there's more to maggot therapy then an ace bandage and a few upended trashcans. You need to know what you're doing, and not just any maggot will do.
Advertisement