There's a fungus among us, and it's making us miserable. The culprit is part of the genus Trichophyton. It belongs to a class of fungi called dermatophytes and lives in the epidermis, or the outer layer of skin, where it dines exclusively on the protein keratin. Keratin is tough: It's a major component in skin (as well as horns and claws in other animals), where it helps keep out germs and other foreign invaders.
Trichophyton is among a relative handful of microbes equipped with the enzyme needed to break down keratin's fibrous composition. Obligingly, you turn out new epidermal cells every four weeks, providing the fungus with an endless, all-you-can-eat feast.
Advertisement
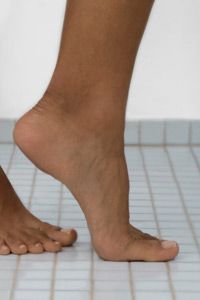
Like other fungi, Trichophyton thrives in warm, moist areas. On the human body, that's primarily the scalp, groin and feet. Infection by Trichophyton is called tinea, from the Latin word for larva. Infected patches sometimes resemble the holes that moth larvae gnaw in woolen clothing. From this resemblance comes its common English name, ringworm.
Ringworm takes other names, some of them even more descriptive, depending on the body part infected. A general outbreak is calledtinea corporis, ringworm of the body. If it occurs on the scalp, it's tinea capitis, ringworm of the head. In the groin or buttocks, the condition is called tinea cruris, better known as jock itch. An infection of the foot is tinea pedis -- which is casually called athlete's foot.
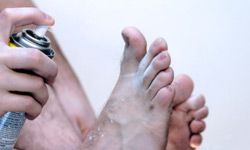
While no worms are involved in ringworm, it may make you feel like you're being munched on by moths. Your skin turns red and scaly. It cracks, peels and itches. Infected nails can crumble and separate from their beds. Bald patches can open on the scalp.
How does Trichophyton find its way to your skin? How can you prevent it from settling in -- or, failing that, get rid of it? What happens if you don't? Where can you get relief?
Advertisement