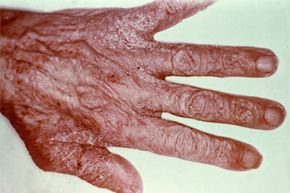
You're lying in bed at night when you suddenly feel an itch on your leg. Without giving it much thought, you reach down and scratch. No big deal, right? But in the morning, your small itchy spot has turned into an angry-looking rash, and it's even itchier. Is it just some weird allergic reaction, or could it have come from a parasite?
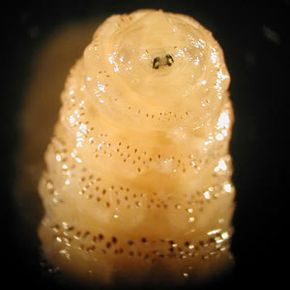
Skin parasites are generally small insects, worms or other bugs that feed on blood or other bodily material. These creepy-crawlies usually fall into one of two categories: external or internal. External parasites tend not to hang around for very long. Most of them either jump on and off, or they leave once they've had their fill. Other parasites try to stick around for longer periods of time. Internal skin parasites burrow under the skin to feed, lay their eggs and make a temporary home for themselves.
Advertisement
Some skin parasites spread between people or other animals, but you can also pick them up from just being in a particular environment. While getting a skin parasite is often more of a nasty nuisance than anything else, a few of these critters can cause some real problems. But the good news is that you can generally prevent a skin parasite infestation by avoiding certain areas or activities, using appropriate insecticides and wearing protective clothing.
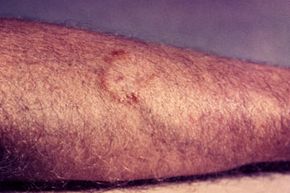
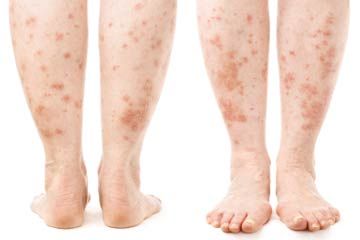
So how can you tell whether that itchy rash was caused by a skin parasite? There are a few general symptoms. First, you have an itchy, crawling feeling on or just under your skin. You might also experience biting, stinging or other pain associated with your rash. The rash might be streaky or could consist of pustules that look a little bit like acne. Also, with many skin parasites, basic over-the-counter treatments for itching don't take care of the problem. If you don't think that you've come in contact with anything else that might cause a rash, it could be time to get to a doctor so you can get the proper treatment.
In this article, we'll learn all about some of the most common skin parasites and how our perceptions of them have changed over the years. Let's start by looking at a very common external skin parasite that afflicts both man and his best friend -- the flea.