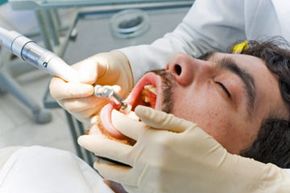
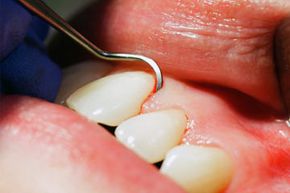
Blood just doesn't belong on a toothbrush, and seeing it there after brushing is more than a little unsettling. Having bad breath not long after brushing your teeth is another discouraging situation. Soreness, sensitivity and loose teeth? Nothing feel-good there, either. All these signs point to gingivitis or periodontitis, two types of gum disease, and no matter whether the symptoms started today or months ago, it's time to take action both offensively and defensively. Teeth and gums are codependent; they have to be all over each other in order to have a healthy relationship. Anything that gets in the way of this bond can be toxic, literally, and a falling out can lead to a real loss -- of the relationship and even the teeth.
Gum disease is just that, a disease, which means that the gum tissues are not working the way they're supposed to within the design of the body; they're in a state of decline. Normal gums are typically pink, smooth and moist, with seamless connections to teeth. Vessels and nerves supply blood flow and sensations to the entire mouth and this circulation allows gums to remain firmly committed to holding tight to the teeth, keeping them straight, immobile and ready to do the work of chewing necessary for digesting food.
Advertisement
When gums suffer neglect or attack from plaque left on or between teeth or from sickness or hormonal changes in the body, gingivitis starts to settle in. Gingivitis is an early form of gum disease that starts to impair the relationship between the teeth and gums. Technically, gingivitis is gum inflammation. Periodontitis is a much more serious form of gum disease involving inflammation around the entire tooth and it can lead to the breakdown of gums, their supporting tissues and even the bones beneath [source: NIH]
Both periodontitis and gingivitis are gum disease, but they are different in the degree of damage they do. Advanced gum disease leads to increased bacteria and toxins, along with active infections, and the body's immune system kicks in to fight them. Unfortunately, it also turns on itself by annihilating gum tissues and bone in the process: To fight the disease, the body defends itself by attacking infection, and the connecting tissues and bone around the teeth get "taken out" in the process. It is this loss of support that can lead to tooth loss [source: NIH].
How can you tell when your gums, teeth and immune system are at odds with each other and disease has set in? Sometimes you can't, but we'll look at some obvious rifts in the relationship, next.
Advertisement