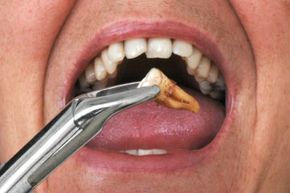
While teeth whitening may be the most requested cosmetic dental procedure in America, flashing a smile of pearly whites takes more than just bleach -- good oral hygiene is key to a healthy mouth.
Who among us, though, hasn't suffered a cavity? As it turns out, most of us have. Ninety-two percent of American adults ages 20 to 64 have had at least one cavity in their permanent teeth [source: NIDCR]. That's a lot of dental fillings. Left untreated, even just a small spot of decay can turn ugly. Sometimes, damage and decay is severe enough that it can't be repaired with a filling, crown, root canal or other restorative treatment, and then extraction comes into the picture. When a tooth is extracted, it's permanently removed from the mouth. Teeth that are infected are also recommended for removal -- while oral antibiotics will clear a bacterial infection that has spread to the jaw, those antibiotics can't take the fight inside of a tooth where the infected nerve is. Removing the tooth removes the decay and infection, preventing the spread of infection and inflammation to other areas of the mouth and body.
Advertisement
Teeth that are loose or that no longer have surrounding supportive bone and soft tissue are also common candidates for extraction, as are impacted wisdom teeth. When wisdom teeth -- our third molars -- don't have enough room, they can become impacted, which means they're stuck in the jaw and can't erupt. Wisdom teeth may also sometimes only partially erupt, usually because of crowding in the mouth as well. Impacted wisdom teeth may cause pain, swelling and other complications if not removed.
Tooth extractions are also sometimes performed on an elective basis. For example, extractions are sometimes done in preparation for other dental procedures or orthodontic treatments such as braces. Cancer patients and organ-transplant patients have an increased risk of developing infections and may have teeth extracted before or after treatment if those teeth pose a risk for or develop infection during treatment or recovery.
And sometimes, it just comes down to individual anatomy: Some people just have too many teeth for the size of their mouth, and teeth are extracted to ease crowding.
Now you know many of the reasons why a tooth may need to be removed, but did you know there is more than one type of extraction? Let's dive more deeply into extraction, from prep to procedures.
Advertisement