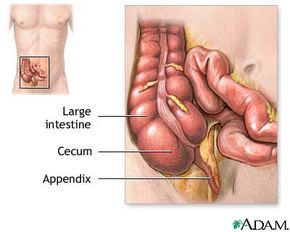
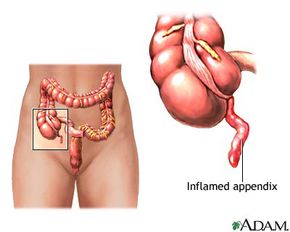
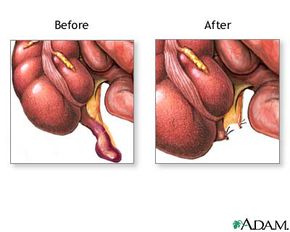
Location, location, location. You've likely heard this phrase thrown around in the real estate world, but the truth is it can be used to describe the appendix, too. Except here's the problem: The appendix is in a bad neighborhood. The location of the appendix is at the cecum -- the beginning of the colon where the small and large intestines join -- which places it in a prime spot for infection. The appendix resembles a closed end tube with an opening in the middle that can allow fecal matter to enter, so it's easy to see how an infection in the appendix can quickly develop and become a health emergency. The appendix is only about 3 or 4 inches long, so why all the trouble from such a small organ?
Here's another head-scratcher -- the appendix doesn't appear to have any function in the human body. Scientists theorize that the appendix is a remnant of an ancient digestive tract. They believe that it might have been used by early man to digest tough leaves and bark.
Advertisement
Because doctors don't really know the purpose of the appendix, they're unable to determine what system it belongs in. It's a simple structure that's made up of two types of tissue. The outside of the appendix is muscle tissue, but given the lack of activity, the muscle is considerably weaker than the muscle tissues that make up other organs. The lining of the appendix is filled with lymphatic tissue, which produces antibodies, leading many to believe that the appendix may be part of the immune system. Another odd characteristic of the appendix: It manufactures and secretes a small amount of mucus. No doubt about it, the appendix is confusing.
Of course, it's understood that the human body functions perfectly well without the appendix, but some scientists are still unwilling to declare the appendix useless.
So what is appendicitis, anyway? And what's really happening when an appendix bursts? Find out on the next page.
Advertisement