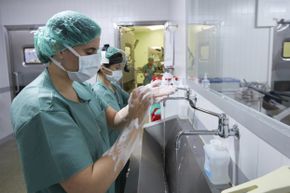
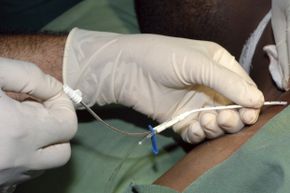
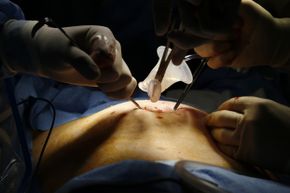
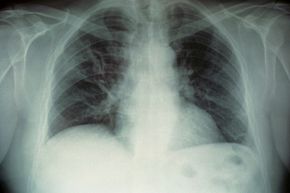
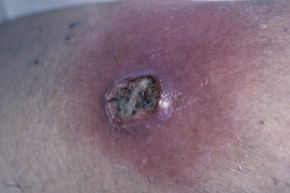
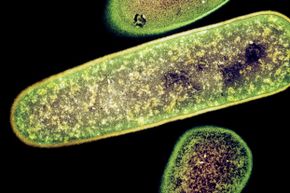
When we're sick, really sick, most of us will head for the hospital, but sometimes that stay can lead to another illness on top of that first medical issue. These hospital-acquired infections (also known as health care-associated infections or nosocomial infections) occur because a hospital puts a lot of people with infections in one place, many of them with compromised immune systems. Without strict procedures for maintaining sterile conditions, pathogens can spread.
One in 25 hospital patients contracted an HAI in 2011, according to a Centers for Disease Control and Prevention survey of U.S. hospital data. Overall, that worked out to an estimated 722,000 such infections that year, and 75,000 of those patients died, although not necessarily from the HAI) [source: CDC].
Advertisement
This article explains which infections are most common, how they're spread and what health care facilities are doing to prevent them.