There are around 17 million people in America who woke up this morning, shuffled into the bathroom, looked at themselves in the mirror and yelled, "Aw, come on!" Then, many of them started scrubbing, washing, peeling and picking at their faces in their attempts to rid themselves of their acne.
Most of these acne sufferers are teenagers and twentysomethings. However, the good times don't always end with the passing of adolescence -- adults get acne, too. In this cruel world, even babies get it. At some point in our lives, most of us will experience the unpleasantness of acne.
Advertisement
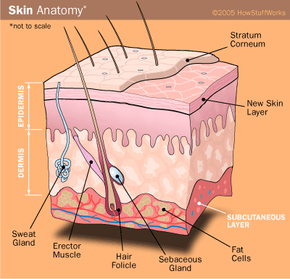
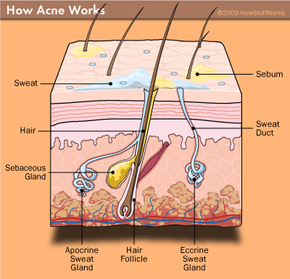
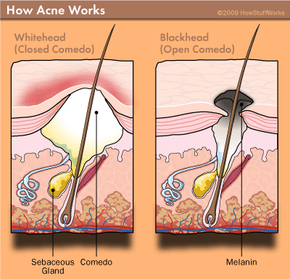
Acne can take many forms, which we'll discuss in this article: whiteheads, blackheads, pimples and even large, cystlike masses. It's caused essentially by the blocking of one of the hair follicles in your skin. As infection deepens and pressure grows behind this clog, a pus-filled bump forms on top of your skin -- the dreaded pimple. In a moment, we'll take a more in-depth look at how your skin functions when things are running smoothly (and not-so-smoothly).
We know how acne forms -- and why some conditions, namely rosacea, cause acne -- but opinion varies on how to treat it. In this article, we'll learn what acne is, what causes it, how to prevent it from appearing in the first place and how to get rid of it after it shows up. In addition to some more traditional methods, such as washing with benzoyl peroxide or taking antibiotics, we'll look at the latest weapons in the war on acne, such as lasers and isotretinoin. So, if you're an acne sufferer, keep your chin up. And if you can't, we'll hopefully teach you some ways to get rid of that giant chin pimple that's weighing you down.
Advertisement