You haven't been near poison ivy in weeks, you aren't allergic to latex and you don't have allergies that give you hives -- at least, you don't think you do. So what's that red patch of itchy dry skin? It could be a type of eczema. An estimated 15 million Americans are affected by it [source: EczemaNet]. The name eczema is actually an all-encompassing title for a range of skin conditions that produce the same itching and redness, the most common of which is called atopic dermatitis (or atopic eczema).
Atopic dermatitis is the most common type of eczema found in infants and children under the age of two. In fact, about 10 to 20 percent of infants have eczema [source: UVA Health System]. The disease occurs less frequently in adults, but they can still be affected through periodical flare-ups that are triggered by different allergic reactions or reactions to skin irritants.
Advertisement
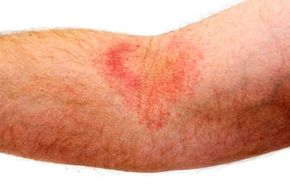
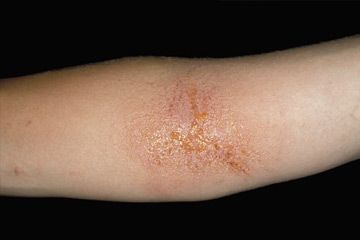
The symptoms of atopic dermatitis are overshadowed by one major characteristic -- itchiness. Atopic dermatitis is almost always itchy; it can be itchy even before a rash appears, and scratching can both cause and worsen the rash. In babies, eczema most often occurs on the face, arms, legs, scalp and neck. In children and adults, it usually shows up in the folds of elbows and knees. Skin affected by eczema can appear dry, thickened and scaly. Fair-skinned people who have the condition may have reddish patches of skin that turn brown, while dark-skinned people can experience changes in pigment that either darken or lighten the affected skin [source: WebMD].
Other diseases grouped under the label of eczema include:
- Contact dermatitis, which is caused by the skin being exposed to irritants or allergens
- Nummular dermatitis, which consists of coin-sized patches of affected skin and is usually found in adults Hand eczema, which causes a rash on the hands
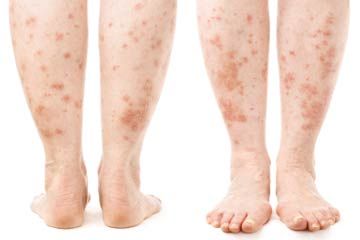
- Stasis dermatitis, which appears on the calves, ankles and feet of people who have poor blood circulation
- Seborrheic dermatitis, which affects the scalp and may cause dandruff in adults
[source: InteliHealth]
Similar factors cause these types of eczema, and you treat most of them in similar ways. Read on to find out more about what can cause those itchy red patches.
Advertisement