The human body isn't a perfect organism and, by extension, neither is any surgery. That goes for dental implants as well. Designed to replace a lost tooth (or teeth), dental implants have become increasingly popular -- and for good reason. They offer a permanent solution for patients, and the track record for successful dental implant surgery is impressive. Still, there are a number of potential complications that you should be aware of prior to having the work done, or even post-surgery.
While the risk of complications is considered to be very low -- less than 5 percent, according to current statistics -- there's a much greater likelihood that you might be a candidate for dental implants. According to the American Association of Oral and Maxillofacial Surgeons, almost 70 percent of adults between the ages of 35 and 44 have lost "at least one permanent tooth to an accident, gum disease, a failed root canal or tooth decay" [source: AAOMS].
Advertisement
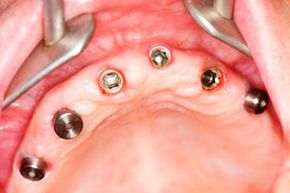
Just two decades ago, the options for a lost tooth were much more restricted. Patients typically would get either removable dentures that rested on the gums (a favorite among old hockey players), or a fixed bridge that anchored to adjacent healthy teeth. Neither were ideal solutions. Dental implants -- where the replacement structure is bolted, often with a titanium screw, directly to the patient's jawbone -- give oral surgeons a promising option to restore teeth permanently. The implant fuses with the jawbone in a process called osseointegration to provide the same solid connection that a natural tooth has (and sometimes stronger). A fitted crown is then attached to the implant to complete the procedure.
But dental implants aren't always the perfect solution. Potential problems include infection, insufficient bone mass, incorrect positioning, fractured implants, damage to surrounding tissue (including gums, nerves and blood vessels) and teeth, overloading and even reaction to anesthesia.
Though the vast majority (more than 95 percent) of all dental implant procedures are completed without complication, it's wise to be aware of what can go wrong, since a rapid response to any problem will enable surgeons to take corrective actions. Most problems are minor and easily rectified. However, if left untreated, even minor problems can threaten the long-term viability of the implant.
Keep in mind that all is not lost if a dental implant fails. Surgeons can usually attempt a second implant, either immediately or within several months after the area has sufficiently healed. Timely assessment is key.
What are the risks of infection with implants?
Advertisement